Smoking and vaping
Last Modified 14/05/2026 15:42:41
Share this page
Introduction
Smoking remains the leading cause of preventable death in England, responsible for an estimated 74,600 deaths in 2019.1 It is also the largest contributor to health inequalities, accounting for around half the difference in life expectancy between the most and least deprived communities.2 These figures emphasise its continuing significance as a major public health challenge. More recent national estimates of smoking-attributable mortality are not yet available due to the COVID-19 pandemic and a revised methodology to produce updated figures is being developed by the Office for Health Improvement and Disparities (OHID).
Facts and figures
Smoking prevalence in Blackpool
In England there has been a steady decline in smoking prevalence in the adult population, with a reduction from 19.8% in 2011 to 11.6% in 2023. The picture in the North West as a whole is similar to England with smoking prevalence following a similar trend. In Blackpool, there was a decline from 28.1% in 2011 to 20.6% in 2023. The decline was steady until 2016 but has since fluctuated, with progress slowing and rates remaining significantly higher than the national average (figure 1).
Figure 1: trend in smoking prevalence in adults aged 18 and over - current smokers (one-year range) proportion, Blackpool and England
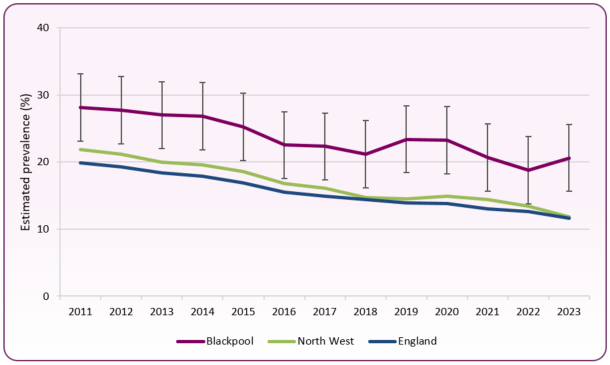 Source: OHID, Smoking Profile
Source: OHID, Smoking Profile
During the coronavirus pandemic, changes to data collection methods likely resulted in an underestimate of adult smoking prevalence in 2020, as reported by the usual source, the Annual Population Survey (APS). These figures should therefore be interpreted with caution. In contrast, the online Opinions and Lifestyle Survey (undertaken by the Office for National Statistics) provided a consistent estimate of smoking prevalence during this period. From this, smoking prevalence among those aged 16 and over in Great Britain fell by 1.3% in 2020 compared with 2019, although this decrease was not statistically significant. Note: the APS measures smoking prevalence in those aged 18 and over, so the two sources cannot be directly compared.
Smoking prevalence and deprivation
Many local authorities with the highest smoking rates continue to be among the most deprived in England. In 2021, smoking prevalence was 23.8% in the most deprived areas - nearly four times higher in the least deprived areas( 6.8%).3 Although smoking has declined across all groups, this stark inequality remains. This inequality is reflected in respiratory health outcomes: in 2021-23, the most deprived decile had a chronic obstructive pulmonary disease (COPD) mortality rate over twice that of the least deprived (69.8 vs 29.7 per 100,000).4
Figure 2 shows the distribution of current smokers in England by deprivation decile, where decile 1 represents the most deprived 10% of areas and decile 10 the least deprived. In 2021, over two-fifths (43.3%) of all smokers lived in the two most deprived deciles, compared with 14.8% in the two least deprived deciles. Helping disadvantaged smokers to quit and preventing smoking uptake in deprived communities remain key strategies to reduce health inequalities, particularly in Blackpool, where deprivation is among the highest in England, and smoking rates remain disproportionately high.
Figure 2: smoking prevalence by deprivation indices: England, 2021
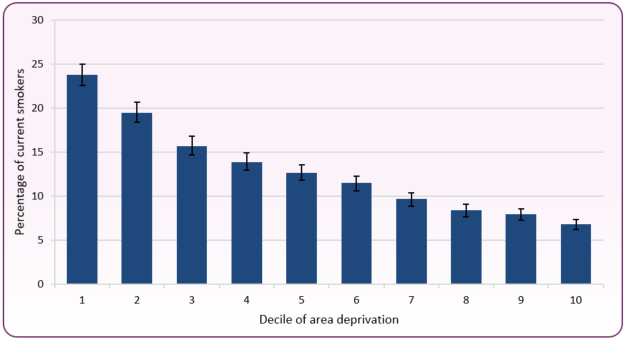 Source: Office for National Statistics (ONS), deprivation and the impact on smoking prevalence, 2017-21Please note, this is based on the 2019 Index of Multiple Deprivation (IMD) and produced by the Office for National Statistics, there is no information if or when an updated version based on the 2025 IMD will be published.
Source: Office for National Statistics (ONS), deprivation and the impact on smoking prevalence, 2017-21Please note, this is based on the 2019 Index of Multiple Deprivation (IMD) and produced by the Office for National Statistics, there is no information if or when an updated version based on the 2025 IMD will be published.
Smoking prevalence and health inequalities
Smoking remains the leading cause of health inequalities in England, contributing to around half of the difference in life expectancy between the most and least affluent communities. As previously noted, it is strongly associated with indicators of disadvantage, and although national smoking prevalence continues to decline each year, the gap between the most and least deprived groups has widened, with reductions occurring more slowly in more deprived areas.
In 2022/23, 25.1% of adults aged 18 and over in England with a long-term mental health condition reported that they currently smoked. For Blackpool the proportion was 43.6%, significantly higher than England. The likelihood of smoking is significantly higher among those with a mental health condition; in 2022/23, adults with a long-term mental health condition were 3.3 times more likely to smoke than those without. Although smoking is perceived to be stress-relieving, research shows that mental health does not worsen as a result of quitting smoking, and is in fact associated with reduced levels of anxiety and depression.5 Partly a result of high smoking rates, people with a mental health condition have high mortality rates compared to the general population. Therefore, quitting smoking is particularly important for this group since smoking is the single largest contributor to their 10-20 year reduced life expectancy.
Analysis of data collected in England between 2013 and 2019 shows that smoking prevalence declined more rapidly among lesbian and gay adults compared to heterosexual adults, such that rates were similar by 2018–2019. However, bisexual men and women remained significantly more likely to smoke than heterosexuals, even after adjusting for factors such as age, ethnicity, and socioeconomic status. Bisexual smokers also showed lower levels of nicotine dependence, with fewer cigarettes smoked per day and a lower likelihood of smoking soon after waking. There were no significant differences between sexual orientation groups in motivation to quit, quit attempts, or quit success. These findings highlight that while inequalities in smoking narrowed for lesbian and gay adults over the study period, bisexual people continued to experience higher smoking rates and may benefit from targeted tobacco control interventions.7
Looking at ethnicity for England, smoking prevalence was higher among adults of a mixed ethnic background (17.0%) compared to the national average (12.7%) (2022). Smoking rates were lower than average among Chinese (8.4%), Asian (7.4%), and Black (4.7%) ethnic groups. Between 2011 and 2022, the percentage of adults who smoked has broadly followed a trend of decline across all ethnic groups.8
The smoking rate for adults (18-64) in routine and manual occupations in Blackpool (23.5%) is statistically similar to England (19.5%). The trend does show a reduction in both local and national proportions. Smoking prevalence by economic activity status varies. Those defined as unemployed had a higher proportion of current smokers (19.7%), compared with those who were in paid employment (11.4%) and those who were economically inactive (12.2%).9 The local economy in Blackpool has historically been shaped by tourism but the decline of the seaside resort industry has contributed to sustained levels of unemployment and economic inactivity above the national average. This economic landscape likely plays a role in sustaining higher smoking prevalence locally, reflecting the strong association between unemployment and smoking observed nationally.
Smoking during pregnancy/smoking status at time of delivery (SATOD)
Smoking during pregnancy can cause serious pregnancy-related health problems and have detrimental effects on the development of the baby and health of the mother. Statistics on smoking during pregnancy and women's smoking status at time of delivery (SATOD) are available on the dedicated Blackpool JSNA Smoking in Pregnancy page. Smoking during pregnancy and exposure to secondhand smoke can lead to premature birth, low birth weight and poor infant health. For the period 2020-22, Blackpool's premature birth rate (less than 37 weeks gestation) of 106.8 per 1,000 births is significantly higher than the national rate of 77.0. In 2022, 3.1% of term babies in Blackpool had a low birth weight (below 2.5kg), similar to England (2.9%).
Smoking-related mortality
Figure 3 shows the estimated rate of deaths per 100,000 of the population, aged 35+, that are attributable to smoking. In 2017-19 this equated to around 1,000 deaths in Blackpool at a rate of 379.9 per 100,000 population, significantly higher than the national average (202.2 per 100,000) and the third highest rate in the country. Whilst smoking-attributable mortality has been gradually falling in England and the North West, numbers and rates in Blackpool have remained relatively steady.
Figure 3 - trend in smoking attributable mortality, Blackpool, North West and England
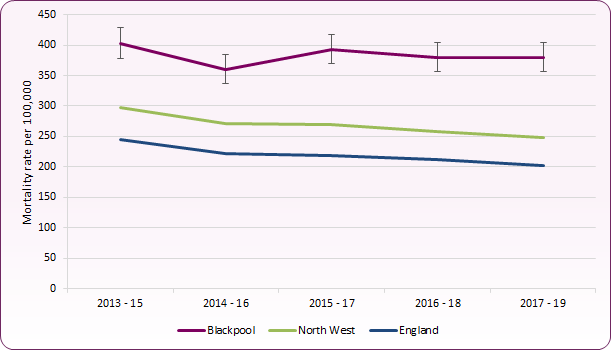 Source: OHID, Smoking Profile
Source: OHID, Smoking Profile
A breakdown of smoking-attributable deaths and mortality rates for smoking-related disease provides a more detailed understanding of the impact of smoking on mortality (figure 4). Smoking-attributable deaths from cancer, heart disease and stroke are all significantly higher than England. Mortality rates for lung cancer, oral cancer and chronic obstructive pulmonary disease (COPD) are also significantly higher than the national rates. Smoking-attributable deaths for stroke and heart disease were the second and third highest rates in the country respectively. Blackpool's mortality rate for COPD rose steadily from 68.3 per 100,000 in 2007-09 to 102.6 per 100,000 in 2016-18, and after a drop to 77.5 in 2019-21, has since risen to 83.4 (22021-23).
Figure 4: smoking-attributable deaths and mortality rates (per 100,000) from smoking-related disease
| Smoking-attributable deaths | Blackpool | England |
|---|
| Number | Rate | LA rank (1=worst) | Rate |
|---|
| Heart disease (2017-19) |
157
|
59.7
|
1
|
29.3
|
|---|
| Stroke (2017-19) |
42
|
16.2
|
2
|
9.0
|
|---|
| Cancer (2017-19) |
376
|
142.7
|
7
|
89.6
|
|---|
| Mortality rate | Number | Rate | LA rank (1=worst) | Rate |
|---|
| Lung cancer (2021-23) |
350
|
76.4
|
8
|
47.5
|
|---|
| Oral cancer (2020-22) |
38
|
8.5
|
6
|
5.2
|
|---|
| COPD (2021-23) |
382
|
83.4
|
3
|
43.9
|
|---|
Source: OHID, Smoking Profile
Blackpool also has the highest estimated level of 'potential years of life lost' (PYLL) due to smoking-related illness, with a 2016-18 rate of 2,819 per 100,000, compared to the England average of 1,313.
Smoking-related ill-health and smoking-attributable hospital admissions
Blackpool has the highest rate of smoking-attributable hospital admissions of any local authority in the country. This indicator aims to quantify the scale of preventable hospital admissions due to smoking-related conditions. This is indicative of poor population health and high smoking prevalence. Blackpool has seen a rise in smoking-attributable hospital admissions, from 2,528 per 100,000 in 2015/16 to 3,071 per 100,000 in 2019/20 (figure 5).
Figure 5: trend in smoking-attributable hospital admissions, Blackpool, North West and England
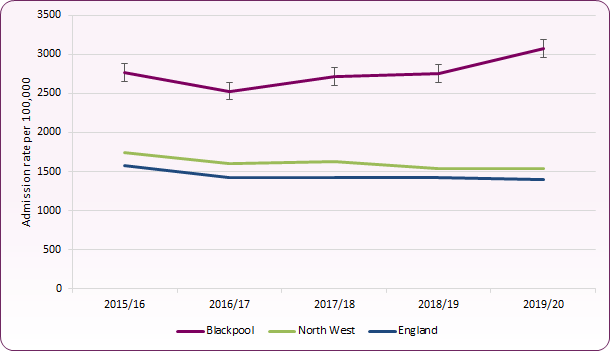 Source: OHID, Smoking Profile
Source: OHID, Smoking Profile
Smoking-related hospital registrations for lung, oral, and oesophageal cancers (all 2017-19) and COPD emergency hospital admissions (2023/24) are significantly higher than England averages and are among the highest in the country (figure 6).
Figure 6: Smoking related hospital registrations and admissions - numbers and rates (per 100,000 pop.)
| Registration/admission condition | Blackpool | England |
|---|
| Number | Rate | LA rank (1=worst) | Rate |
|---|
| Lung cancer registrations (2017-19) |
484
|
111.7
|
15
|
77.1
|
|---|
| Oral cancer registrations (2017-10) |
104
|
24.2
|
3
|
15.4
|
|---|
| Oesophageal cancer registrations (2017-19) |
99
|
23.0
|
2
|
15.2
|
|---|
| COPD emergency admissions (2023/24) |
668
|
724
|
7
|
357
|
|---|
Source: OHID, Smoking Profile
Societal costs of smoking in Blackpool
The total burden caused by tobacco products more than outweighs any economic benefit from their manufacture and sale. Action on Smoking and Health (ASH) provide estimates of the cost of smoking to Blackpool. According to the 2023 Ready Reckoner (based on 2022 prevalence data), the economic cost of smoking in Blackpool is estimated at £73.7 million per year. This includes:
-
-
£7.7 million in healthcare costs (hospital admissions and primary care)
-
£5.3 million in social care costs (residential and domiciliary care)
-
£1.5 million in fire costs (deaths, injury, property damage, and fire & rescue)
-
£59.3 million in productivity losses (lost earnings, unemployment, and early death)
Vaping and electronic cigarettes
Electronic cigarettes, or vapes, deliver nicotine through a vapour rather than through tobacco smoke. Since their introduction to the UK market in the early 2010s, vaping has grown significantly in popularity, both as a smoking cessation aid for adults and, increasingly, as a recreational activity among young people.
The long-term health effects of vaping, particularly for young people who have never smoked, are not yet established. The prevalence of vaping among children and young people in Blackpool, and across the UK, has become a significant public health concern, as demonstrated in the Children and Young People’s Vaping Report for Blackpool. Blackpool’s position remains that vaping should be used as a short-term quit aid for adult smokers.
This section examines the current data on the health impacts, vaping prevalence, legislation, and services in Blackpool.
Health concerns associated with vaping include:
-
-
Nicotine addiction, particularly in young people whose brains are still developing
-
Respiratory issues, including coughing, wheezing, and exacerbation of asthma
-
Potential cardiovascular effects
-
The ‘gateway effect’: concern that vaping may lead to smoking, particularly among young people11
There are approximately 4.7 million e-cigarette/ vape users in the UK, with 9.1% of adults in Great Britain currently using e-cigarettes (2023 data). Most adult e-cigarette users, 56%, are ex-smokers, with vaping primarily used as a smoking cessation tool. However, 37% of current adult vapers also smoke (dual users). 6.7% of current e-cigarette users say they have never smoked. However never smokers make up the majority of the adult population, which equates to 1.1% of never smokers who are current vapers.
Vaping use among children and young people
| Survey/study | Key findings |
|---|
| GB Youth Survey on vaping among 11–17-year-olds in Great Britain (2025), ASH |
7% of 11-17-year-old currently vape. 5% of 11-15-years. 12% of 16-17-years and 15% of 18-year-olds.
20% of 11-17-year-olds had tried vaping in 2024 – unchanged since 2023.
Current vape use (11–17): 49% of current smokers; 27% of former smokers; 4.2% of never smokers (up from 0.1% in 2013).
Dual use (smoke + vape): increased from 0.6% (2014) to 2.8% (2025)
|
|---|
| NHS England: Smoking, Drinking and Drug Use among Young People in England - NHS England Digital |
5% of 11-15-year-olds are regular e-cigarette users; 4% are occasional users.
18% of 15-year-olds had tried vaping; 19% were current users (11% regular, 8% occasional).
A higher proportion of girls reported both current use and having ever used e-cigarettes.
|
|---|
| HealthWatch Blackpool Children and Young people’s Vaping Report (2023) |
Prevalence: 31% of young people vape; 40% of vapers do so daily; 75% use disposables. Access: easily bought from corner shops, friends, or family; sellers rarely check ID. Social influences: Social media, advertising, and peers promote vaping. Risks: many underestimate harms; some users report side effects (nosebleeds, coughing). Knowledge gaps: Many unaware of laws (eg puff limits, under-18 sales) or nicotine risks. Education: Young people want better, more impactful education about health risks.
|
|---|
| Schools Health Education Unit (ages 12-15) (2024) |
Ever vaped: 41% of 12–15-year-olds (47% in 2022).
Regular use (≥ weekly): 12% of 12–15-year-olds
|
|---|
Blackpool trading standards is responsible for enforcing age-of-sale legislation, tackling illegal sales of vaping products, and ensuring compliance with the ban on disposable vapes, which should negate some of the environmental harms of vapes/e-cigarettes. These impacts include plastic and electronic waste, fire risks from lithium batteries, and low levels of recycling.
National and local policies
Local strategies
Tobacco FREE Lancashire: Towards a Smokefree Generation 2023-2028  (1887Kb)
(1887Kb)
The Tobacco Free Lancashire strategy has the overarching framework of Smokefree – to reduce the damaging impact of tobacco by helping people to quit smoking, reducing the availability of illicit tobacco and challenging the social norm of smoking. It is seeking to create more smokefree environments and spaces across communities and challenge the norm of smoking.
The Tobacco Free Lancashire strategy was developed in line with the Smokefree 2030 ambition, the NHS Long Term Plan (2019), NICE guidance (2021), the 2017 – 2022 Tobacco Control Plan, and recommendations from the 2022 Khan Review. It also reflects emerging national policies from 2023.
It sets out the ambition to achieve the smokefree ambition of lowering smoking prevalence to less than 5% in every neighbourhood by 2030 through:
-
- preventing children from taking up smoking in the first place
- stamping out inequality for example smoking in pregnancy
- supporting smokers to quit
The strategy has prioritised the following areas based on detailed local intelligence in order to reduce health inequalities and improve quality of life by reducing smoking prevalence in the following groups: pregnant women, people with mental health conditions, and people with long-term conditions.
The Blackpool Smokefree Alliance has developed a bespoke action plan for the local area, informed by a Blackpool-specific CLEAR assessment. Local partners meet quarterly to implement and review progress against key priorities.
The Directors of Public Health position statement on nicotine vaping September 2023  (1550Kb) has been produced collaboratively by the public health directors across Lancashire and South Cumbria, it represents the agreed position of public health with regard to nicotine vaping.
(1550Kb) has been produced collaboratively by the public health directors across Lancashire and South Cumbria, it represents the agreed position of public health with regard to nicotine vaping.
The position statement accepts the priority should be on tobacco control, but acknowledges the significant concerns around vaping including the use by children and the health risks; easy access to vapes as well as the direct and indirect advertising/ marketing of the products; the rise in availability of illicit products; the environmental impacts of single-use vapes; the role of vapes in helping adults to quit smoking; and the urgent need to provide clarity to NHS provider services and settings on the status of vapes in NHS Smokefree Policies. In Blackpool, Blackpool Teaching Hospitals NHS Foundation Trust enforces a blanket Smokefree policy, in place since 2007, which prohibits both smoking and vaping across all Trust premises, including buildings, entrances, grounds and car parks.
Healthwatch Blackpool, Smoking and Vaping. For Healthwatch Blackpool’s collaboration with Public Health Blackpool and NHS Smokefree Blackpool Tobacco Addiction Treatment Service, insights were gathered from adults, children and young people who smoke or vape, including recent starters, those who had relapsed, and the wider community. The aim was to understand the behaviours of people who smoke or vape, as well assessing the effectiveness of the NHS Smokefree Blackpool Tobacco Addiction Treatment Service (Oct 2025).
National strategies
The World Health Organisation Framework Convention on Tobacco Control remains the overarching international treaty guiding tobacco control. Earlier national strategies such as the NHS Long Term Plan (2019) and the Department of Health’s 'Towards a Smokefree Generation: A Tobacco Control Plan for England' (2017) set the direction for reducing smoking and improving cessation support.
The 2017 plan introduced the concept of a smokefree generation, defined as reducing adult smoking prevalence to 5% or lower, and set interim goals to 2022. It did not set a specific target date for achieving smokefree status but stated that work would continue beyond 2022. The government formally adopted the 2030 target for a smokefree England in its Advancing our health: prevention in the 2020s Green Paper (2019).
The Khan Review assessed progress towards the 2030 target and recommended measures, including raising the age of sale of tobacco, investing in stop smoking services, and regulating vaping to protect young people. These recommendations informed the UK Government’s Smokefree Generation policy, announced in 2023, which proposes banning the sale of tobacco to anyone born on or after 1 January 2009, to first take effect in January 2027. This policy is detailed in the Stopping the Start: Plan to Create a Smokefree Generation (2023), which Blackpool Council supports. The ban on disposable vapes, introduced under the ‘Stopping the Start’ plan by the Conservative government, has since been implemented, and the Labour government has maintained support for the smokefree ambition, continuing to legislate the remaining measures - including restrictions on flavours, packaging, and free samples - set out in the 2023 plan.
The NICE guideline, Tobacco: preventing uptake, promoting quitting and treating dependence, first published in 2021 and updated in 2025, continues to provide evidence‑based recommendations and quality standards for health, public health, and social care. The review also recognised Cytisinicline as an additional cessation aid for 2025 - a medicine made from plants that helps people stop smoking by reducing cravings and making cigarettes feel less satisfying.
The Fit for the Future: 10 Year Health Plan for England (2025) embeds smoking and vaping control within its wider prevention agenda, building on earlier strategies such as the Stopping the Start plan (2023) and the NHS Long Term Plan (2019). It reaffirms commitments to the smokefree generation target, the ban on tobacco sales to anyone born on or after 1 January 2009, and tighter vaping regulations. It also introduces new measures, including:
-
- Additional funding for local stop-smoking services and enforcement.
- The full national rollout of lung cancer screening for smokers; preoperative smoking cessation requirements.
- New digital support tools, such as the NHS Health Coach and AI-guided advice, to help people quit smoking and vaping.
The plan’s focus on targeted support, prevention, and reducing health inequalities is particularly relevant to Blackpool, where smoking prevalence remains high and contributes significantly to poor health outcomes. Effective local delivery of these national measures will be key to addressing the entrenched inequalities and demand on NHS services seen in the area.
Smoking services in Blackpool
- Blackpool has one of the highest smoking-related death rates in England, with persistently high smoking prevalence and significant health inequalities.
- Smoking is concentrated among disadvantaged communities, routine and manual workers, pregnant women, and people with mental health conditions - groups who face greater barriers to quitting.
- Services are designed to be accessible, integrated, and targeted at those most affected, in line with the Tobacco Free Lancashire & South Cumbria Strategy (2023–2028) and priorities identified in the Khan Review (2022).
- While provision is available to all, services also ensure targeted engagement and support for groups with particularly high smoking prevalence as noted above and including people with long-term conditions such as COPD, diabetes, coronary heart disease and asthma.
Community stop smoking services12
Free support provided through clinics, drop-ins, telephone advice, and outreach. Services offer:
-
- Free helpline to speak to an advisor.
- Free nicotine replacement therapy (NRT).
- Harm reduction advice.
- Designed to reach residents in deprived areas who may face barriers to healthcare, providing flexible and convenient support to encourage engagement.
Inpatient Tobacco Dependence Services13
Support is delivered to patients during hospital stays at Blackpool Teaching Hospitals. Hospitalisation is used as a ‘teachable moment’ to motivate quitting, as highlighted in local strategy and practice. It Includes:
-
- Screening all inpatients for smoking status.
- Immediate access to NRT and behavioural advice.
- Referral to community services for follow-up after discharge.
Maternity smoking services14
Maternity-specific contact number and email address. Specialist stop-smoking support is embedded in maternity care. This includes:
-
- Carbon monoxide screening offered to all pregnant women as part of routine antenatal care.
- Regular behavioural support and free NRT.
- Ongoing support during pregnancy and after birth.
- Addresses high rates of smoking in pregnancy, improving outcomes for mothers and infants and reducing intergenerational smoking.
Support for NHS Staff
Free stop-smoking support available for all staff at Blackpool Teaching Hospitals NHS Trust. This includes:
-
- Free NRT.
- Ongoing support from the same team that supports patients.
- Supports NHS staff, many of whom come from the same high-risk local communities, and helps set a positive example for patients.
Smokefree NHS Trust
-
- Blackpool Teaching Hospitals NHS Trust is a fully smokefree site.
- Smoking is not permitted anywhere on trust premises, including entrances, car parks, and grounds.
- This protects patients, staff, and visitors from second-hand smoke and reinforces public health messaging.
References
[] NHS Digital, 2023. Statistics on Public Health: part 2 - mortality 2023. Accessed July 2025.
[] Office for Health Improvement and Disparities (OHID). Smoking and inequalities 2023. Accessed July 2025.
[] Office for National Statistics, 2023. Deprivation and the impact on smoking prevalence, England and Wales 2017 to 2021. Accessed July 2025.
[] OHID. Respiratory disease profile. Accessed August 2025.
[] Taylor G.M.J., Lindson N., Farley A., Leinberger-Jabari A., Sawyer K., te Water Naudé R., Theodoulou A., King N., Burke C., Aveyard P. Smoking cessation for improving mental health. Cochrane Database of Systematic Reviews 2021, Issue 3.
[] OHID, Smoking Profile. Accessed July 2025.
[] Jackson SE, Brown J, Grabovac I, et al. Smoking and quitting behavior by sexual orientation: a cross-sectional survey of adults in England. Nicotine Tob Res. 2021 Jan;23(1):124–134. doi:10.1093/ntr/ntaa042. PMID:32219478; PMCID:PMC7789956. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7789956/
[] Race Disparity Unit. Adult smokers [Internet]. London: Cabinet Office; 2023 [cited 2025 Jul 13]. Available from: https://www.ethnicity-facts-figures.service.gov.uk/health/alcohol-smoking-and-drug-use/adult-smokers/latest/
[] Office for National Statistics, 2024. Adult smoking habits in the UK - Office for National Statistics. Accessed July 2024
[] OHID. Nicotine vaping in England: 2022 evidence update. Accessed July 2025.
[] Balogun B. Youth vaping in England. London: House of Commons Library; 2024 Jan 12. (Research Briefing CBP‑9932). Available from: https://researchbriefings.files.parliament.uk/documents/CBP-9932/CBP-9932.pdf. Accessed July 2025.
[] Blackpool Council public health. Smokefree Blackpool (2025) Stop Smoking Blackpool. Accessed July 2025.
[] Blackpool Teaching Hospitals NHS Foundation Trust. Inpatient Stop Smoking Service. Available from: https://www.blackpoolteachinghospitals.nhs.uk/services/stop-smoking-service. Accessed July 2025.
[] Blackpool Teaching Hospitals NHS Foundation Trust. Smoking and Pregnancy. Available from: https://www.blackpoolteachinghospitals.nhs.uk/services/maternity/smoking-and-pregnancy. Accessed July 2025.