Drug Misuse
Last Modified 25/03/2026 10:14:57
Share this page
Introduction
Drug misuse is a major concern, both locally and nationally, causing harm to individuals, families and communities. The 2020 Independent review of drugs by Professor Dame Carol Black found harms from drug misuse cost society an estimated £9.3 billion per year, 86% of which is attributable to the health and crime-related costs of the heroin and crack cocaine markets. Drug deaths were at the highest level on record; since 2012 heroin-related deaths had more than doubled and deaths involving cocaine had increased five-fold. The highest rates of opiate and crack use were seen in the North of the country and in the most deprived areas.1
Nationally, the UK Government plan 'From harm to hope: A 10-year drugs plan to cut crime and save lives' sets out their ambitions to cut off the supply of drugs by criminal gangs and give people with a drug addiction a route to a productive and drug-free life. Underpinned by record investment of over £3 billion in the next three years, they aim to reduce drug-related crime, death, harm and overall drug use.
Locally, Blackpool addresses the substance misuse needs of the population through a range inter-related strategies and services. In addition to adult drug misuse needs outlined below, please also see the following:
Prevalence of drug use in England and Blackpool
It is not possible to measure the prevalence of drug use across the UK accurately. Prevalence estimates are generated from a range of sources in order to gain a general understanding of patterns of use nationally, regionally and locally.
The ONS Crime Survey for England and Wales (CSEW) is the primary means of estimating drug use prevalence.2 The 2024 survey found for England and Wales:
- An estimated 8.8% of people aged 16-59-years (approximately 2.9 million) reported using any drug in the past 12 months (2023/24), no significant change compared with 2023.
- Overall, 3.0% of people (approximately 1,000,000) had used a class A drug in the past 12 months - no significant change from 2022/23.
- 1.8% of people were frequent drug users (more than once a month), which is a decrease from the previous year (2.3%).
- Drug use is highest in young adults; an estimated 16.5% of people aged 16 to 24 years reported any drug use in the past 12 months compared to 7.2% of people aged 25 to 59 years.
- The prevalence of drug use has fallen in people aged 16 to 24 years, from 21.0% in 2020, largely as a result of falls in cannabis use in this age group (from 15.4% in 2022/23 to 13.8% in 2023/24).
- More males aged 16-59 used any drug (10.7%) compared to females (7.0%).
- Cannabis has consistently been the most used drug in England and Wales; 6.8% of people aged 16-59 years report using the drug, with the highest reported use in males aged 16-24 (15.1%).
- While there has been a one percentage point decrease in the use of cannabis for those aged 16 to 59 years when compared with 2020, levels are almost six percentage points lower for those aged 16 to 19, and four percentage points lower for those aged 20 to 24.
- For those aged 30 to 34 there has been a slight increase from 2020 of one and a half percentage points in cannabis use.
- For most individual drug types, there were no significant changes in use compared with 2020 (those aged 16-59).
- Significant differences are seen in the use of hallucinogens (increase from 0.7% to 1.2%), ecstasy use decreasing from 1.4% to 1.2% and amphetamine use reducing from 0.3% to 0.2%. Nitrous oxide use has also decreased from 2.4% to 0.9%.
- Those with household incomes of less than £10,400 per year were more likely to use any drug in the last year (12.3%), and in particular cannabis (10.7%), than those with higher incomes.
- A friend, neighbour or colleague was the most common source of illegal drugs (48.9%), not significantly different to 2022/23 (45.7%). The next most common source of illegal drugs was a known dealer, with 11.2% of people reporting that they obtained the drug this way. Almost a fifth (18.4%) said they did not wish to answer the question.
- The most common sources of nitrous oxide or new psychoactive substances (NPS) were a friend, neighbour or colleague (37.8%) or a shop (14.8%).
Drug use prevalence varies by age group, with younger age groups having higher levels of overall drug use prevalence (any illicit substance) (figure 1). For 2024, the estimated proportion of people reporting any drug use in the last year was higher among younger age groups (16.5% of those aged 16 to 24 years) compared with older age groups (7.2% of those aged 25 to 59 years). The fall in drug use among those aged 16 to 24 years compared with the year ending March 2023, was mostly seen in males and females using cannabis (from 16.5% to 15.1% for men and from 14.2% to 12.5% for women). In contrast, there was a slight increases in drug use among those aged 55 to 59 years only (3.1% to 3.6%) compared with 2023.
Figure 1: CSEW estimated drug prevalence by age group, England and Wales 1997 to 2024
 Source: Office for National Statistics, Drug Misuse Appendix Tables: Findings from the year ending March 2024 Crime Survey for England and Wales.
Source: Office for National Statistics, Drug Misuse Appendix Tables: Findings from the year ending March 2024 Crime Survey for England and Wales.
ONS regional estimates suggest that in North West of England for the year up to March 2023:
-
-
9.9% of adults aged 16 to 59 had taken a drug in the previous year. The other highest estimated rates were in the South East (10.1%) and Wales (9.9%)
-
3.5% of adults had taken a Class A drug
- 2.4% of adults had taken powdered cocaine, a decrease from 3.6% in 2019
-
Estimated prevalence rates for all substances in 2024 are lower than pre-Covid (2019/20) except hallucinogens (0.2% to 1.1%) and cannabis (7.3% to 7.6%).
Coronavirus and drug prevalence
There are suggestions that COVID-19 lockdown periods altered patterns of drug use, both as a consequence of changes to behaviour during lockdown and because of the impact on global supply chains. A 2020 survey by Release3 suggested, for example, that there may have been reduced use of MDMA / ecstasy during the COVID-19 period (due to restrictions on night-time economy / social activity), whilst cannabis use was common. The report also suggested that as well as harms from coronavirus itself, the COVID-19 period brought additional risks for some people who use drugs, with increased frequency of (non-fatal) overdose, withdrawal problems, increased police contact, and the sharing of injecting equipment.
Opiate and crack use prevalence in Blackpool
Local prevalence data is not available from the CSEW. However, for the 2019/20 period, the Office for Health Improvement and Disparities (OHID) and the UK Health Security Agency (UKHSA) have estimated the number and prevalence of opiate and/or crack cocaine use (OCU) based on revised methodology.4 Information about OCU is an essential part of the evidence base to help plan services to tackle opiate and crack dependence. OCU does not include the use of cocaine in powder form, amphetamine, ecstasy or cannabis.
In 2019/20, 2,468 people (aged 15-64) were estimated to be using opiate and/or crack cocaine in Blackpool, a crude rate of 28.6 per 1,000 population. This compares to a rate of 9.5 per 1,000 for England and 11.9 per 1,000 for the North West. Blackpool’s estimated OCU rate was the third highest in the country after the City of London (56.8) and Middlesbrough (31.3), and remains the same as the previous estimate in 2018/19.
For opiate use only it is estimated there were 1,182 opiate users in Blackpool (2019/20) at a rate of 13.7 per 1,000 population, and the fifth highest in the country. There were an estimated 310 crack cocaine users, at a rate of 3.6 per 1,000 population (fourth highest in country). Drug treatment data in itself is not a reliable measure of prevalence, however service data suggests that since 2016-17 there has been a slight increase in opiate users also using crack cocaine (and a reduction in opiate users not using crack cocaine). This may be indicative of a changing trend in use.
Ketamine use
Ketamine is a widely used human and veterinary medicine indicated as a dissociative anaesthetic and analgesic agent and, more recently, prescribed for the management of treatment-resistant depression.
Ketamine misuse has been recognised internationally since the 1970s and in the UK since the 1990s, when it became popular as a club drug. Most users have typically used the drug intermittently, although a minority use the drug more frequently and are at greater risk of long-term adverse effects.
Ketamine is commonly misused in an illicit context, where it is taken for its rapid onset dissociative effects, including a feeling of detachment from surroundings.
There is increasing evidence of users consuming ketamine to self-treat underlying physical or mental health disorders, including pain, anxiety and depression. Ketamine use can also lead to these disorders, resulting in a vicious cycle of escalating use.
The peak age group for reported ketamine use in the UK is 20 to 24 years, although there is considerable use in people younger than this, including school-aged children and university students. People of mixed or multiple ethnicity or who self-identify as gay, lesbian or bisexual are more likely to report ketamine use than the general population aged 16 to 59.
Of particular concern, longer-term ketamine use is associated with several chronic adverse effects, which can be debilitating and life-changing and persist despite treatment. These effects may not resolve, or only partially resolve, if ketamine use is discontinued. The risk of these effects is often not understood by users until damage, sometimes irreversible, has been done. Longer-term ketamine use causes dependency and significant adverse effects on the bladder, upper urinary tract, kidneys, abdomen, liver and bile ducts.
There has been a substantial increase in overall ketamine use since 2010, especially involving younger people, accompanied by evidence of increasing regular high-dose use, ketamine dependence and associated health harms. Data from the Crime Survey for England and Wales (CSEW) indicates increasing numbers of people aged 16 to 59 who reported using ketamine in the last year, from 117,000 (0.4% of this population) in the financial year 2012/2013 to a peak of 299,000 (0.9%) in 2022/2023. There was a larger proportionate increase in last year use for those aged 16 to 24 from 52,000 (0.8%) in 2012/2013 to 222,000 (3.8%) in 2022/2023).5
Research undertaken with the Blackpool community and health professionals reveals the disturbing rise of ketamine use among Blackpool’s young people. The study highlights the need for creative, youth-centred, and co-produced interventions that embeds the lived experience of ketamine users, their friends, family members, and carers.
-
- General substance misuse guidelines and harm reduction strategies do not address unique psychological and physical risks, including bladder damage, dissociation, dependency patterns, or pain management.
- Blackpool’s ketamine crisis is a “perfect storm” of affordability, accessibility, and peer-driven normalisation.
- Blackpool could be a national frontrunner in the ketamine response, demonstrating that progress emerges through coordinated, data-informed, and collaborative approaches.
Drug offences among over-18s in Blackpool
Police recorded drug offences may not be a reliable measure of overall drug prevalence since they take place within a specific legislative framework, are subject to particular policing strategies and resources (e.g. locally targeted initiatives), and may also reflect illicit drug use that is more detectable. Offence data can, however, offer an insight into the type of offences taking place locally and any emerging trends in substances in use.6
The data looked at offences recorded for the four main drug types (cannabis, cocaine, heroin, and crack). Between April 2024 and March 2025, 60% of offences for possession of a controlled drug among over-18s in Blackpool was for cannabis, whilst 17% were for cocaine and 6% for heroin. This compares to 68% cannabis, 14% cocaine and 3% heroin across the wider Lancashire Constabulary area for the same period. Almost three-quarters (74%) of all recorded drug offences in Blackpool were for possession (76% across Lancashire).
For possession with intent to supply offences, 29% involved cocaine, 28% crack, 14% involved cannabis, and 14% heroin. Across Lancashire 31% of possession with intent to supply offences involved cannabis, 29% cocaine, 14% crack and 11% heroin. 12% of all recorded drug offences across Blackpool and 18% across Lancashire were for possession with intent to supply.
Supplying, or offering to supply, a controlled substance comprised 8% of all drug offences in Blackpool during 2024/25 compared to 6% across Lancashire. 46% of these offences involved crack, 27% heroin, 10% cocaine and 6% cannabis. For Lancashire this was 28% for cocaine, 20% for crack, 19% for cannabis, and 19% for heroin.
5% of drug offences in Blackpool and Lancashire during 2024/25 involved the production of, or being involved in the production of, cannabis.
Drug-related harm: drug deaths
Drug related deaths are categorised into deaths relating to drug poisoning and a subset of these relating to drug misuse. Deaths from drug misuse are recorded where a drug controlled under the Misuse of Drugs Act 1971 was mentioned on the death certificate and the cause of death is related to poisoning by drugs, assault by drugs or mental disorders related to volatile substances.2
Drug related deaths are a significant cause of premature mortality in the UK and have been on an upward trend over the past decade. This is driven primarily by deaths involving opiates, though also from increases in deaths involving other substances such as cocaine.
In 2022-2024, 14,754 drug poisoning deaths were registered in England (8.8 deaths per 100,000 population), an increase from 14,157 in 2023 and the highest number since records began in 1993. Of these 66% (9,789) deaths were related to drug misuse (5.8 per 100,000). The male drug misuse death rate of 8.4 is over twice the female rate of 3.3 (both per 100,000).
The highest rate of drug misuse deaths was found in those aged 40-49 years. They are part of the age cohort often referred to as "Generation X", born between the late 1960s and early 1980s who have consistently had the highest rates of drug misuse for the past 25 years. The average age at death for drug misuse deaths in 2023 was 44.5 years for males and 47.5 for females. The average for males has been increasing since the late 1990s and is now at a historic high, while the average for females has been relatively consistent over the last 30 years.
Almost half (46.8%, 2,551 deaths) of all drug poisoning deaths in England and Wales involved an opiate, though deaths involving cocaine have also risen significantly over the last 10 years (1,118 deaths in 2023 compared to 139 in 2012). Over half of all drug-poisoning deaths also involve more than one drug, and it is not possible in those cases to tell which substance was primarily responsible for the death. In recent years the number of deaths associated with potent synthetic opioids (nitazene or fentanyl) is causing concern, with a new data collection from OHID reporting 179 deaths across England between June 2023 and May 2024.7
Blackpool facts and figures
Blackpool continues to have the highest drug-related death rates in the country, with 128 deaths from drug poisoning between 2022 and 2024, a rate of 32.4 per 100,000 population (directly standardised rate). The death rate is almost four times higher than England, 8.8 per 100,000 (figure 2). There were 83 deaths from drug misuse which account for almost two-thirds (65%) of the drug poisoning deaths in Blackpool.
-
- Of the drug misuse deaths in 2022-24, over two-thirds (59, 71%) were male, 24 (29%) were female
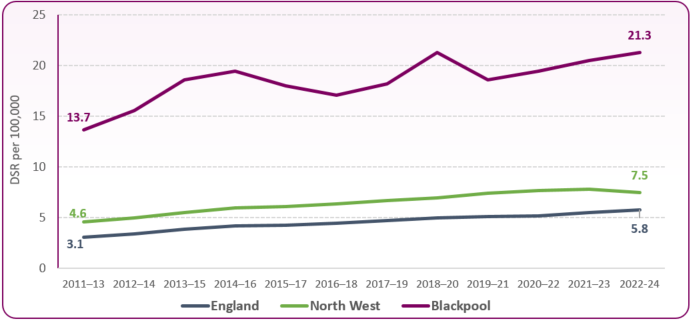
- The drug misuse death rate in Blackpool for all persons is 21.3 per 100,000, almost four times higher than the England rate of 5.8 per 100,000. The rate has increased by 37% over the last 10 years from 15.6 in 2012-14 (England’s rate has increased by over 70% over the same period, up from 3.4 to 5.8)
- The second highest rate in England, to Blackpool, is Gateshead, 14.2 per 100,000
Whilst national and regional rates increased during the COVID-19 affected period (2019-21), Blackpool's rate fell from 21.3 per 100,000 in the 2018-2020 period to 18.6 in 2019-2021 (figure 2). This was due to the number of deaths from drug misuse reducing from 28 or 29 each year between 2018 and 2020, to 18 in 2021. However, rates are once again increasing.
Figure 2: deaths from drug misuse, Blackpool, North West and England, 2011-13 to 2022-24 (rate per 100,000 population)
 Source: Office for National Statistics (ONS) Drug misuse in England and Wales: year ending March 2024
Source: Office for National Statistics (ONS) Drug misuse in England and Wales: year ending March 2024
In Blackpool the death rate has decreased for males, while the female rate has increased (figure 3).
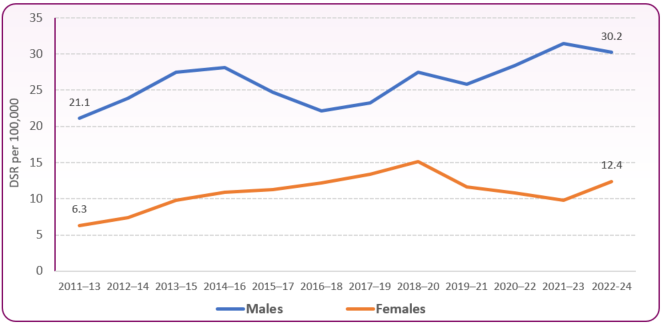
- The death rate for males in Blackpool is almost four times higher than England, 30.2 per 100,000 compared to 8.4. This is the highest rate in England, with Gateshead and Chesterfield having the second highest (21.7)
- The female death rate is four times higher than England, 12.4 per 100,000 compared to 3.3, and is now the highest rate, with Liverpool having the second highest (9.5)
Figure 3: deaths from drug misuse, Blackpool males and females, 2011-13 to 2022-24 (rate per 100,000 population)
 Source: Office for National Statistics (ONS) Drug misuse in England and Wales: year ending March 2024
Source: Office for National Statistics (ONS) Drug misuse in England and Wales: year ending March 2024
Drug-related harms: hospital admissions
NHS Digital reports data for drug-related hospital admissions in three main areas:8
Admissions for drug-related mental and behavioural disorders
The latest available data for 2023/24 show:
-
- There were approximately 20 hospital admissions in Blackpool where the primary reason for admission was a drug-related mental and behavioural disorder.
- Blackpool's hospital admission rate was 14.1 admissions per 100,000, compared to an England rate of 7.7 per 100,000. This was the 20th highest rate among local authorities in England.
- The rate has increased from 11.1 admissions in 2022/23, but has dropped from 2019/20 where the rate was 28.5.
Admissions where drug-related mental and behavioural disorders were a factor in treatment
In addition to the primary reason for admission (above), hospitals collect secondary diagnosis information, where a drug-related mental and behavioural disorder was not necessarily the main reason why a patient was admitted to hospital, but was relevant to the patient's care. In Blackpool during 2023/24:
-
- There were 720 hospital admissions where drug-related mental and behavioural disorders were either the primary reason for admission or were a factor in treatment/care.
- This equates to a crude rate of 534.9 admissions per 100,000 population, compared to 180.9 across England. The Blackpool rate is the third highest in the country and after a reduction in 2022/23 has increased again.
Admissions for poisoning by drug misuse
In Blackpool during 2023/24 there were 50 hospital admissions for intentional and unintentional poisoning involving a substance listed as being controlled under the Misuse of Drugs Act 1971.
-
- The rate of 37.2 admissions (per 100,000) is the seventh highest in the country and over twice the England average of 17.9.
- Admissions for poisoning by drug misuse in Blackpool overall have reduced from 90 admissions in 2019/20 (66.6 per 100,000), although there has been a slight increase between 2022/23 and 2023/24.
Hospital admissions trends can be affected by a range of complex factors, particularly during the COVID-19 pandemic, when hospital presentations and admissions changed significantly. Changes to coding, and protocols for treatment and admission can also affect these statistics, and further exploration of the data is required in order to fully understand the drug misuse admission patterns described above.
Drug-related harms: morbidity and risk groups
Drug misuse can lead to a range of wider health consequences, with some groups at greater risk.
Blood-borne viruses, infection and injecting drug use
Injecting is one of the main causes of health damage related to drug use. People who inject drugs (PWID) are at higher risk of fatal and non-fatal overdose, and the sharing of injecting equipment for drug use is an important contributor to blood-borne virus transmission, including HIV, Hepatitis B and Hepatitis C. People who inject drugs are the group most affected by Hepatitis C in the UK, with over 90% of infections diagnosed in England thought to be acquired through injecting drug use.9
PWID are also vulnerable to a wide range of bacterial infections, as well as other damage to veins and arteries.
The 'Unlinked Anonymous Monitoring (UAM) Survey of HIV and Hepatitis in People Who Inject Drugs' presents annual data across England, Wales and Northern Ireland on PWID who are in contact with specialist services.10 In 2023, 92% of PWID reported injecting heroin, whilst 55% reported injection of crack cocaine. 19% of respondents reported sharing needles and syringes. Nearly a quarter of those who injected drugs reported experiencing a non-fatal overdose and non-fatal overdoses were noted particularly in people aged 25 and over. The proportion of PWID carrying naloxone has increased significantly and 59% of those overdosing had naloxone administered.
The 2023 UK Health Security Agency report 'Shooting Up' found that, in 2021:9
-
- Chronic hepatitis C prevalence continues to decline, but prevention of new and re-infections remains a challenge
- Hepatitis B virus (HBV) remains rare, but vaccine uptake has declined substantially
- HIV prevalence remains low and stable, but outbreaks continue
- Preventable bacterial infections remain a problem
- Injecting risk behaviours have not improved
- Changing patterns of psychoactive drug use remain a concern
- Rates of fatal and non-fatal overdose are at an all-time high
- COVID-19 has had a significant impact on PWID and service provision.
In 2023/24, 6% of all new presentations to the specialist drug treatment service in Blackpool were currently injecting drugs, with a further 11% having previously injected. The vast majority of injecting users (current or previous) were receiving treatment for opiate use, and 21% of new opiate presentations to the service were currently injecting drugs.11
Nationally, there are concerns that the COVID-19 lockdown period was a contributory factor in increases in higher risk behaviours (particularly the sharing of injecting equipment). COVID-19 has had a significant impact on PWID and service provision, and it will be important to monitor any continued impact on the drug user population.
Co-occurring mental health and drug use conditions
Mental health problems are experienced by around 70% of drug users in community substance misuse treatment, with death by suicide also common. Those with co-occurring mental health and drug misuse issues are at higher risk of relapse (both in terms of substance misuse and mental health), can experience barriers to accessing services, and often have wider health and social needs. Tackling co-occurring severe mental health problems and drug use (sometimes referred to as 'dual diagnosis') can be complex, and requires a strong therapeutic alliance and collaborative delivery of care between drug treatment and mental health services.12 13
Data from the OHID Co-occurring Substance Misuse and Mental Health Issues Profile suggests that 64.0% of new presentations to the drug treatment service in Blackpool during 2023/24 had concurrent contact with mental health services. This was significantly worse than the national level of 74.5%. In the same period, treatment services identified that 4% of those entering drug treatment in Blackpool were identified as having behavioural or emotional treatment needs, lower than the England average, 17%.
Parental substance misuse is a significant public health concern. The 2003 'Hidden Harm' report by the Advisory Council on the Misuse of Drugs (ACMD) estimated that there were between 200,000 and 300,000 children in England and Wales where one or both parents had serious drug problems. Parental drug misuse can compromise children's health and development from conception onwards, though the risks of harm may be reduced through treatment and support for the affected adult, and by the presence of at least one other consistent parent or carer, a stable home with adequate finances, maintenance of family routines and activities, and regular attendance at a supportive school.14
Parental substance misuse (PSM) is the third most common reason (after domestic abuse and parental mental ill health) children are referred to children’s social care. The experiences of children living with PSM are complex and risk factors are multiple. The challenges experienced have been compounded by the decade-long impact of austerity measures, which have reduced early intervention services, resulting in practitioners prioritising the needs of younger children to the detriment of older children. The research has highlighted the impact of PSM on older children with their increased risk of significant harm due to criminal exploitation and/or child sexual exploitation.15
In 2021 19.9% (560) of all Blackpool's Children in Need assessment episodes identified drug misuse by the parent as a factor. Nationally, 15.5% of assessments identified parental drug misuse as a factor in Children in Need episodes.
Based on data from the National Drug Treatment Monitoring Service (NDTMS), 22% of the 1,390 people in drug treatment in Blackpool in 2023/24 were living with children. There were approximately 255 parents who were living with children, with around 180 of those receiving treatment for opiate use. A further 250 of those in treatment were parents who were not living with children (175 opiate users), and 55 (50 opiate users) were not a parent but were living in a property with children present. The proportion of opiate users in treatment who were living with children is similar to national levels (figure 4).
Source: NDTMS. Note: NDTMS numerical data is rounded to the nearest 5 to prevent patient identification. Proportions are rounded to nearest whole percentage point, and as a result may not total 100%. Drug treatment includes opiates only, non-opiates only, and non-opiate and alcohol.
In addition to parental drug use, parental alcohol misuse is also a concern - see the Alcohol section for further information.
Drug treatment
Specialist drug and alcohol treatment services for adults (and young people) are commissioned by the local authority. In Blackpool adult services are provided by 'Horizon', a partnership between Delphi Medical and Acorn Recovery Projects, together with Renaissance UK and Blackpool Council. Services for children and young adults under-25 are provided by Blackpool Adolescent Service. Information about drug and alcohol treatment services is compiled nationally through the National Drug Treatment Monitoring System (NDTMS).
People in treatment
In Blackpool in 2023/24 there were 1,390 people in drug treatment. Of these 970 (70%) were in treatment for opiate use, 70 (5%) for crack (no opiate) use and 235 (17%) for non-opiate use. Blackpool has a higher proportion of opiate users than is seen nationally (England 63%).
Overall numbers in treatment in Blackpool have remained relatively steady since 2014/15, having fallen by 34% over the first half of the 2010s decade. This was primarily due to a reduction in people in treatment for opiate use between 2009/10 and 2014/15 (figure 5). A similar trend was seen nationally over this period, though the reduction was around 11%. There has been a slight increase in those being treated for non-opiate use from 2020/21 to 2023/24.
Figure 5: trend in numbers in drug treatment by substance type, Blackpool 2009/10 to 2023/24 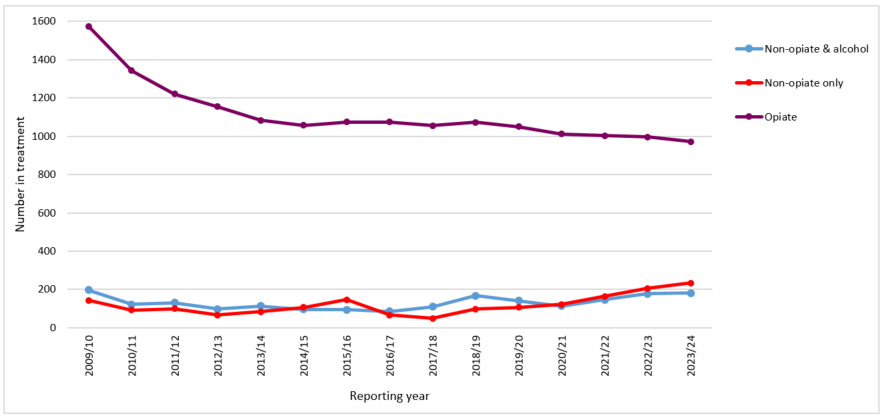
Source: NDTMS, adults in treatment for drug misuse
It was estimated that Blackpool has significantly more adults in treatment than nationally. In 2023/24 the crude rate of those in drug treatment (excluding treatment for alcohol only) was 1,203.3 per 100,000 adult population, compared to 669.4 per 100,000 in England. The crude rate of those in treatment for opiate use was 843.3 per 100,000, almost three times the England rate of 297.1 per 100,000.
Over two-thirds (69%) of those in drug treatment are male, compared to 72% nationally. Blackpool has a higher proportion of female opiate users within treatment (33%) compared to the national average (27%). These numbers have remained relatively stable over the past ten years, although males have seen a slightly bigger decrease than females.
97% of those in treatment identified their ethnicity as white, this is higher than the 2021 Census for Blackpool (90.4% identified as white).
60% of those in drug treatment are aged between 30 and 49 years. Whilst the overall number of 18 to 49 year olds in treatment has been reducing, the number of those aged over 50 increased from 134 in 2014/15 to 367 in 2023/24, and over 50s now account for 26% of the Blackpool treatment population (figure 6). This increase is primarily due to an ageing opiate user population across the country. This cohort tend to have more complex needs due to deteriorating physical and mental health, difficulties navigating health and care systems, and stigma associated with substance use.16
Figure 6: trend in numbers in drug treatment by age group, Blackpool 2009/10 to 2023/24 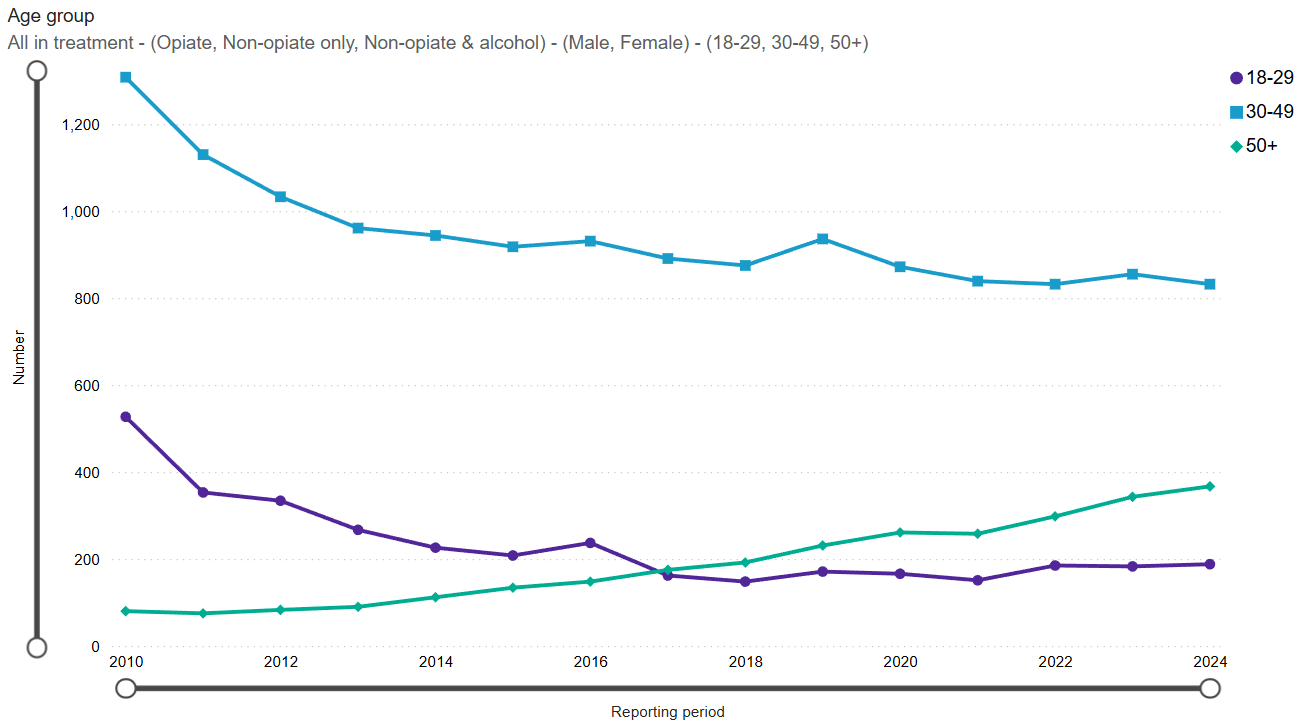
Source: NDTMS, adults in treatment for drug misuse
Source: NDTMS, ViewIt report - figures may not sum due to rounding
Two-fifths (40%) of those in drug treatment have been in treatment for less than two years. 45% (443 people) have been in treatment for four or more years. Most of these are opiate users, highlighting the complex nature of opiate treatment and recovery for many people. The number of those in long-term (4+ years) treatment in Blackpool has risen slightly over the last ten years from 365 in 2012/13.
New presentations
A new presentation to drug treatment services is defined as when a person starts a new treatment journey, either for the first time or returning to treatment having had a break of over 21 days. Information about new presentations to drug services can help to gain insights into current issues and trends relating to drug use and the needs of people who use drugs.
In 2023/24, there were 464 new presentations to the specialist service in Blackpool for drug-related treatment. This is similar to pre-COVID-19 levels showing new presentations to treatment have recovered after the pandemic. New presentations for opiate use have generally been decreasing over the last decade (figure 8), but this has been offset by increases for non-opiate drug misuse. A similar trend is observed nationally, and may reflect changes to drug use, supply and access to services. Overall, 44% of new presentations in Blackpool were for opiate use compared to 40% nationally during 2023/24. Over half (52%) of all new presentations to the service reported opiate and/or crack use, with 32% of these reporting both.
Figure 8: new presentations to specialist drug service by drug type, Blackpool 2009/10 to 2023/24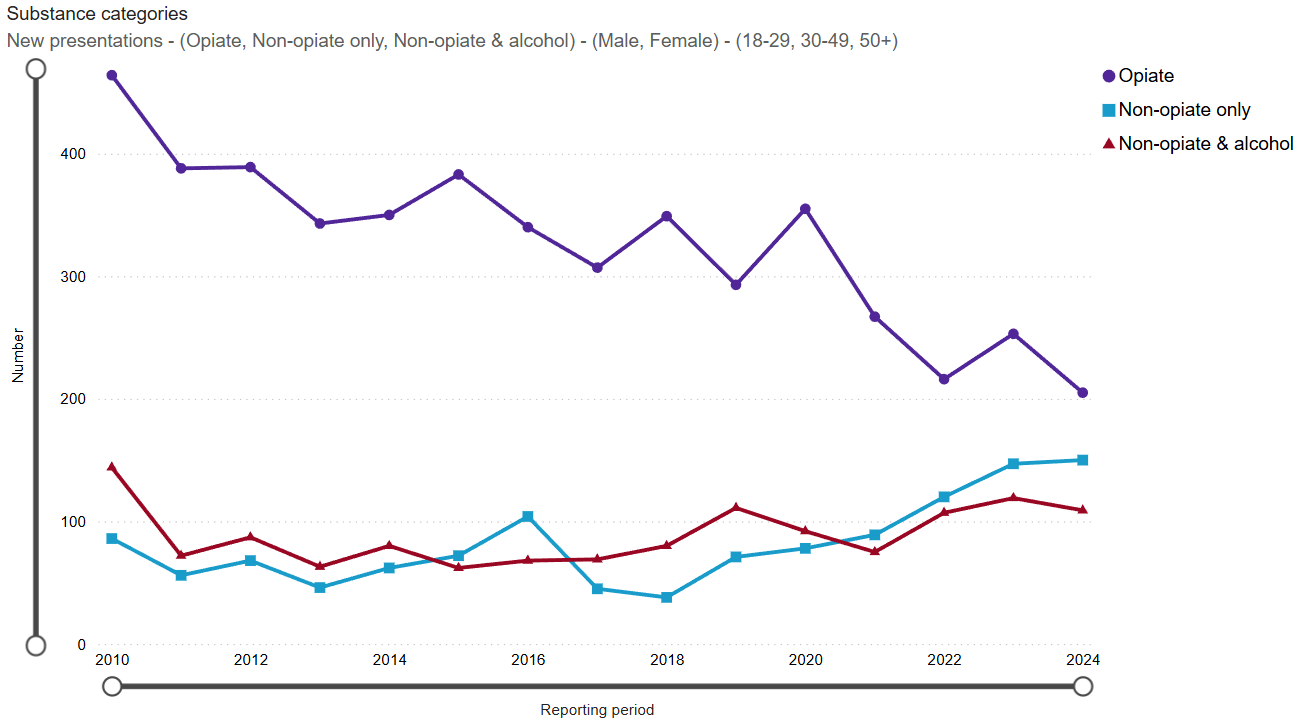
Source: NDTMS, Adults in treatment for drug misuse
As with the overall treatment population, more than two-thirds (70%) of new presentations were male, similar to the national average of 72%. Looking at age breakdown, 58% of new presentations were aged 30 to 49 years, 27% aged 18 to 29 years, and 15% over 50. Blackpool has a similar proportion of presentations in the older age group compared to England (14%).
Wider determinants
Across Blackpool, only 10% of those in drug misuse treatment were in paid work in 2024/25 compared to 21% in England. Just over three-quarters (76%) are in stable and suitable accommodation/housing, compared to 84% in England. Just over a quarter (26%) report having a mental health need and are not receiving mental health treatment (England 19%).
56.5% of referrals to the specialist drug service in 2023/24 were self-referrals or came from family and friends. Other referrals came from criminal justice (21.1%), health and social care (9.9%) and other substance misuse services (4.7%).
Treatment outcomes
The OHID Public Health Outcomes Framework measures a 'successful completion' of treatment as those adults successfully completing and not re-presenting within six months as a proportion of the overall number in treatment for that type of substance.
For opiate users, the percentage of successful completions has been reducing since 2013 (figure 9). Blackpool's completion percentage of 2.9% in 2023/24 is significantly lower than the England proportion of 5.1%. The increase seen in 2021 may have been due due to the impact of COVID-19 on services and treatment.17
Figure 9: trend in successful completion of drug treatment: opiate users, Blackpool and England 2010/11 to 2023/24
 Source: OHID Public Health Outcomes Framework, Indicator C19a
Source: OHID Public Health Outcomes Framework, Indicator C19a
For non-opiate users the percentage of successful completions is significantly greater, in part due to the differences in treatment length between opiate and non-opiate users. In Blackpool in 2023/24, 28.7% of non-opiate users successfully completed treatment, similar to the 29.5% across England (figure 10). The trend of successful completions in Blackpool has generally been falling over the last ten years (as has England's) and has been significantly lower than average in 2018/19, 2019/20, and 2022/23 but is currently in line with the England average.
Figure 10: trend in successful completion of drug treatment: non-opiate users, Blackpool and England 2010/11 to 2023/24
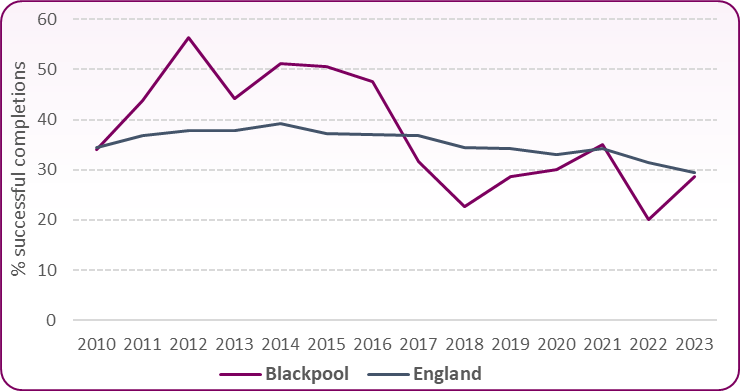 Source: OHID Public Health Outcomes Framework, Indicator C19b
Source: OHID Public Health Outcomes Framework, Indicator C19b
From all the exits from drug treatment for 2023/24, 34% dropped out/left (172 adults aged 18 and over). This compares with 39% across England. The proportion of deaths in drug misuse treatment in Blackpool has remained fairly static over the last four years, with 36 deaths in 2023/24 - 7% of all exits (England 4%).
National and local strategy and response
Following phase two of Dame Carol Black's review of drugs in 2021, the UK Government released From Harm to Hope: A 10-year drugs plan to cut crime and save lives. The plan focuses on three strategic priorities:
-
- Breaking supply chains - focused on preventing drug supply and disrupting gang operations
- Delivering a world-class treatment and recovery system - rebuilding local authorities treatment and recovery services, ensuring service integration, improving access, developing the workforce and improving criminal justice pathways
- Achieving a generational shift in demand for drugs - changing attitudes in society around the acceptability of drug use, applying tougher consequences and delivering prevention and early intervention.
By 2024/25 the UK Government aims to prevent nearly 1,000 deaths and provide at least 54,500 new treatment places, as well as targets to prevent crimes, disrupt organised crime activity and seize criminal assets.
Since the release of the strategy the Government has issued further guidance for local delivery partners, including the publication of a National Combating Drugs Outcome Framework and the establishment of local Combating Drugs Partnerships. The Combating Drugs Partnership will comprise of a range of local partners (including the Local Authority, Police, Probation Service and Integrated Care Board) and will be accountable for delivery against the National Combating Drugs Outcome Framework. In Blackpool, there is a Combating Drugs and Alcohol Board, with the partnership established in 2022.
As an area with high levels of drug misuse and drug-related harm, Blackpool has been a pathfinder site for Project ADDER since 2021. Project ADDER is a joint Home Office and Department for Health and Social Care programme seeking to:
-
- reduce drug-related death
- reduce drug-related offending
- reduce the prevalence of drug use
- deliver sustained and major disruption of high-harm criminals and networks involved in middle market drug / firearms supply and importation
In addition to this, the Blackpool Drug Harm Reduction Strategy 2020-22 set out Blackpool's strategy to reduce the number of people who suffer harm, directly or indirectly, because of the prevalence of drug misuse in the town. The refreshed drug harm reduction strategy (2023-2025) identifies nine strategic priorities to tackle substance misuse. These are around areas such as partnership working, supporting substance misuse services, primary and secondary health care provision, and engaging/supporting people with multiple disadvantage.
As part of the strategy’s response to drug related deaths and non-fatal overdoses, an integrated real time surveillance programme has been introduced across Blackpool. Blackpool Council, Lancashire Constabulary, Horizon Drug Treatment Service and other partners work together to rapidly record and report drug related deaths and non-fatal overdoses, examining contributory factors that might prevent further harms. Lancashire Constabulary have also initiated a drug testing protocol whereby any substances seized at the site of suspected drug related deaths or non-fatal overdoses can be tested for information purposes. Information is shared via Project ADDER to aid response and prevention activity, and any alerts relating to substances of concern are circulated via a Lancashire-wide Local Drugs Information System (LDIS) network.
Naloxone is an opioid antagonist that can be used to reverse the effects of opioids such as heroin, methadone, codeine, morphine, opium and buprenorphine. It can potentially save someone's life in the event of an overdose, though effects don't last very long and medical help is still necessary. Naloxone is used by medical practitioners (including the NW Ambulance Service) and is also available to drug users via the Delphi drug treatment service, Renaissance and Lived Experience. A pilot is commencing in September 2022 to enable police connected to Project ADDER to carry naloxone with a view to extending it to the wider force in future.
[] Black, Dame C. (2020) Review of Drugs - evidence relating to drug use, supply and effects, including current trends and future risks. Home Office, February 2020.
[] Office for National Statistics (ONS) Drug misuse in England and Wales: year ending March 2023
[] Aldridge, J., Garius, L., Spicer, J., Harris, M., Moore, K. & Eastwood, N. (2021) Drugs in the Time of COVID: The UK Drug Market Response to Lockdown Restrictions, London
[] Office for Health Improvement and Disparities and UK Health Security Agency. Estimates of the prevalence of opiate use and / or crack cocaine use. GOV.UK, October, 2023
[] Advisory Council on the Misuse of Drugs, Ketamine: an updated review of use and harms, Updated 28 January 2026
[] Blackpool Council, Blackpool Drug Harm Reduction Strategy Refresh, 2023-2025
[] OHID, Deaths linked to potent synthetic opioids, October 2024
[] NHS England Digital, Statistics on Public Health, England 2023, Part 1- Hospital admissions
[] UK Health Security Agency (UKHSA) (2021) Shooting Up: infections and other injecting-related harms among people who inject drugs in the UK, 2020, and Shooting Up: data tables accompanying the report, update December 2021.
[] UKHSA, Unlinked Anonymous Monitoring (UAM) survey of HIV and viral hepatitis among people who inject drugs (PWID): 2023 report, January 2024
[ ] NDTMS, Substance use and behaviour, ViewIt Report, 2023/24
[] Public Health England (PHE) (2017) Better care for people with co-occurring mental health and alcohol / drug use conditions.
[] National Institute for Health and Care Excellence (NICE) (2016) Coexisting severe mental illness and substance misuse: community health and social care services. NICE Guidance [NG58].
[] Advisory Council on the Misuse of Drugs (ACMD) (2003) Hidden Harm - responding to the needs of children of problem drug users.
[] Todman H, McLaughlin H, (2024) Understanding the Needs of Children Living with Parental Substance Misuse: Perspectives from Children and Practitioners. The British Journal of Social Work, Volume 54, Issue 7. May 2024
[] Advisory Council on the Misuse of Drugs (ACMD) (2019) ACMD report - Ageing cohort of drug users, June 2019.
[] Office for Health Improvement and Disparities (OHID) Adult substance misuse treatment statistics 2020 to 2021: report.