Healthy eating - diet and nutrition
Last Modified 03/04/2024 10:04:58
Share this page
Introduction
Consuming a healthy diet throughout the life course helps prevent malnutrition in all its forms as well as a range of non-communicable diseases and conditions. But the increased production of processed food, rapid urbanisation and changing lifestyles has led to a shift in dietary patterns. People are now consuming more foods high in energy, fats, free sugars or salt/sodium, and many do not eat enough fruit, vegetables and dietary fibre such as whole grains1. The importance of diet as a major contributor to chronic disease and premature death in England is recognised in the Government strategy Tackling obesity: empowering adults and children to live healthier lives. Poor diet is a public health issue as it increases the risk of some cancers and cardiovascular disease (CVD), both of which are major causes of premature death. These diseases, and type II diabetes (which increases CVD risk) are associated with obesity, which has a very high prevalence in England. The costs of diet related chronic diseases to the NHS and more broadly to society are considerable. Poor diet is estimated to account for about one third of all deaths from cancer and CVD.
Current nutrition advice from the NHS advocates balance is the key to a healthy diet. It states eating a wide variety of foods in the right proportions, and consuming the right amount of food and drink will achieve and maintain a healthy body weight. It promotes a diet based on starchy foods such as potatoes, bread, rice and pasta; plenty of fruit and vegetables; some protein-rich foods such as meat, fish and lentils; some milk and dairy foods; and not too much fat, salt or sugar. Figure 1 shows the 'Eatwell Guide' which highlights the different types of food that make up our diet, and shows the proportions we should eat them in to have a healthy, balanced diet.
Figure 1: The 'Eatwell Guide'
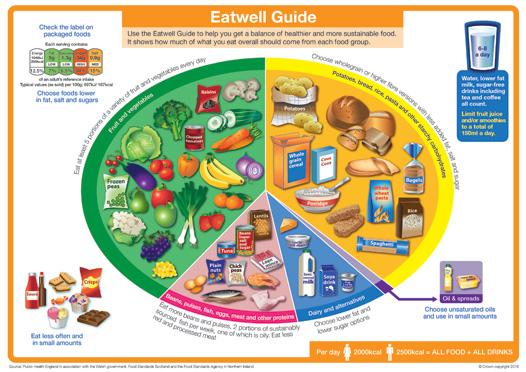 Source: NHS choices, the eatwell guide
Source: NHS choices, the eatwell guide
Food poverty is a growing problem in the current economic climate. The use of food aid in the UK, particularly in the increased use of food banks has dramatically increased. A survey by the Food Foundation found that in June 2023, 17% of households in the UK were 'food insecure' (ate less or went a day without eating because they couldn't access of afford food), up from 8.8% in January 2022. The ability to afford a healthy and sustainable diet is simply out of reach for many people.2 It is estimated that 17% of the UK population live in poverty3.
It is widely reported that individuals and families who experience food poverty are more likely to eat a diet which is unhealthy, characterised by food that is higher in saturated fat, salt and sugar. Additionally, they are more likely to eat processed foods that are both cheap and energy dense. Poor accessibility to affordable healthy foods, linked to a number of factors makes people already vulnerable more susceptible to experiencing food poverty. Factors such as closure of shops in deprived areas, out of town supermarket developments, poor transport links all contribute to poor access and affordability of healthy food.
Facts and figures
Across England we know that:
-
- 7% of households experienced food insecurity in 2020/21. Across the North West it was 8% of households.
- Household food security was lower in households where the head is below the age of 65
- Households with a gross income of less than £200 per week were least likely to be food secure
- Single -adult households with children had low rates of household food security
- Food insecurity is directly associated with poorer diet quality
- Food insecurity is indirectly associated with higher BMI via greater distress and eating to cope
- Just under a third of adults are eating the recommended 5 portions of fruit and vegetables a day
In Blackpool:
-
- A quarter of Blackpool’s children (under 16) live in relative low income families
- 38.6% are eligible for Free School Meals, significantly higher than the national average of 21%
- Blackpool's average weekly earnings of £394 is the lowest in the country
- The proportion of Employment and Support Allowance claimants (12%) is the highest in the country
- Excess weight in adults and children is significantly higher than national averages
- Blackpool has the highest density of fast food outlets in the country (outside the City of London)
Data from the Office for Health Improvement & Disparities (OHID) provides estimates on healthy eating behaviour. Across Blackpool it is estimated that:
-
- 72.3% of adults and 42.3% of children (age 10-11) are overweight or obese4
- 8.6% of the population have been diagnosed with diabetes, significantly higher than the national average
- Less than a third (29.9%) of all adults are eating the recommended 5 portions of fruit and vegetables per day
Figure 2: Percentage of adults aged 16 and over meeting the '5-a-day' fruit and vegetable consumption recommendations, Blackpool compared to UTLAs, England and North West, 2021/22
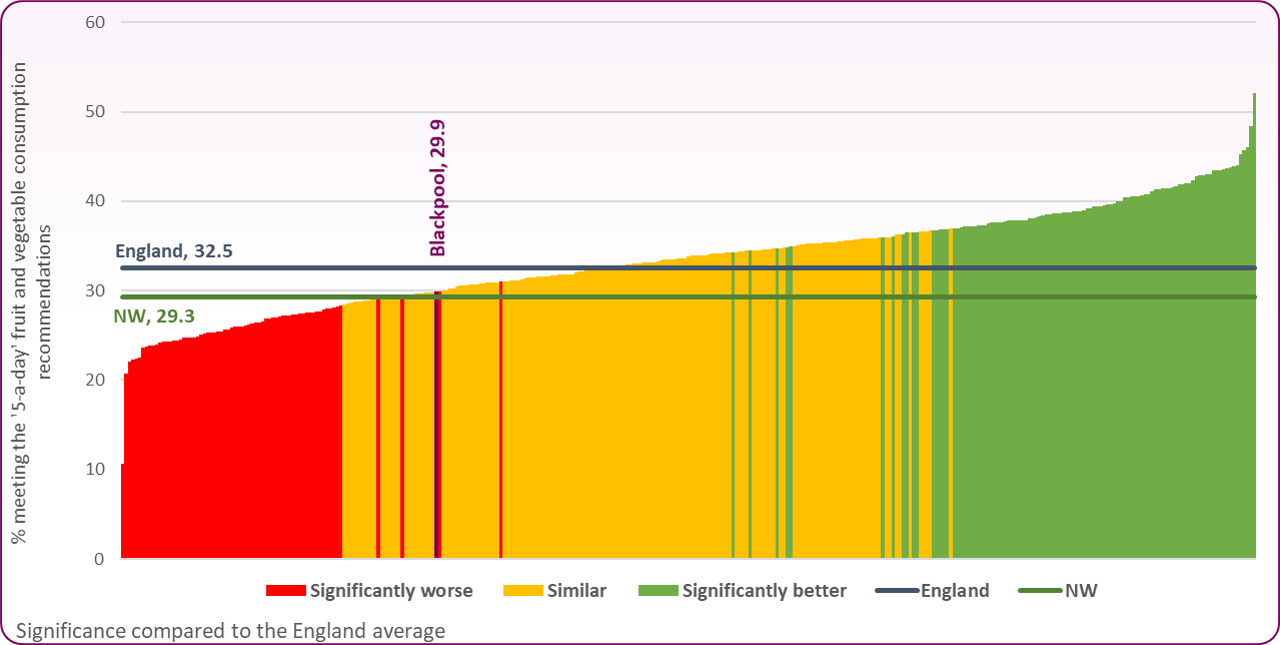 Source: OHID, Obesity Profile
Source: OHID, Obesity Profile
There are many factors which impact on healthy eating and the ability to have a nutritious diet. Key research shows that households/individuals who are in poverty or socially disadvantaged have worse dietary-related outcomes. Food poverty is more likely amongst those who have a low income, are unemployed, have a disability, or are a member of a black or minority ethnic community2. Overall in Blackpool, it is estimated 30% of adults meet the recommended '5 a-day' but Figure 3 shows the inequalites in different sections of the population across England and these inequalities will also occur within Blackpool and supports the findings that healthy eating is less likely in those who are struggling financially, younger people and those with a disability.
Figure 3: Inequalities in the proportion of the England population meeting the recommended '5-a-day' consumption of fruit and vegetables, 2021/22. Blackpool compared to upper tier local authorities
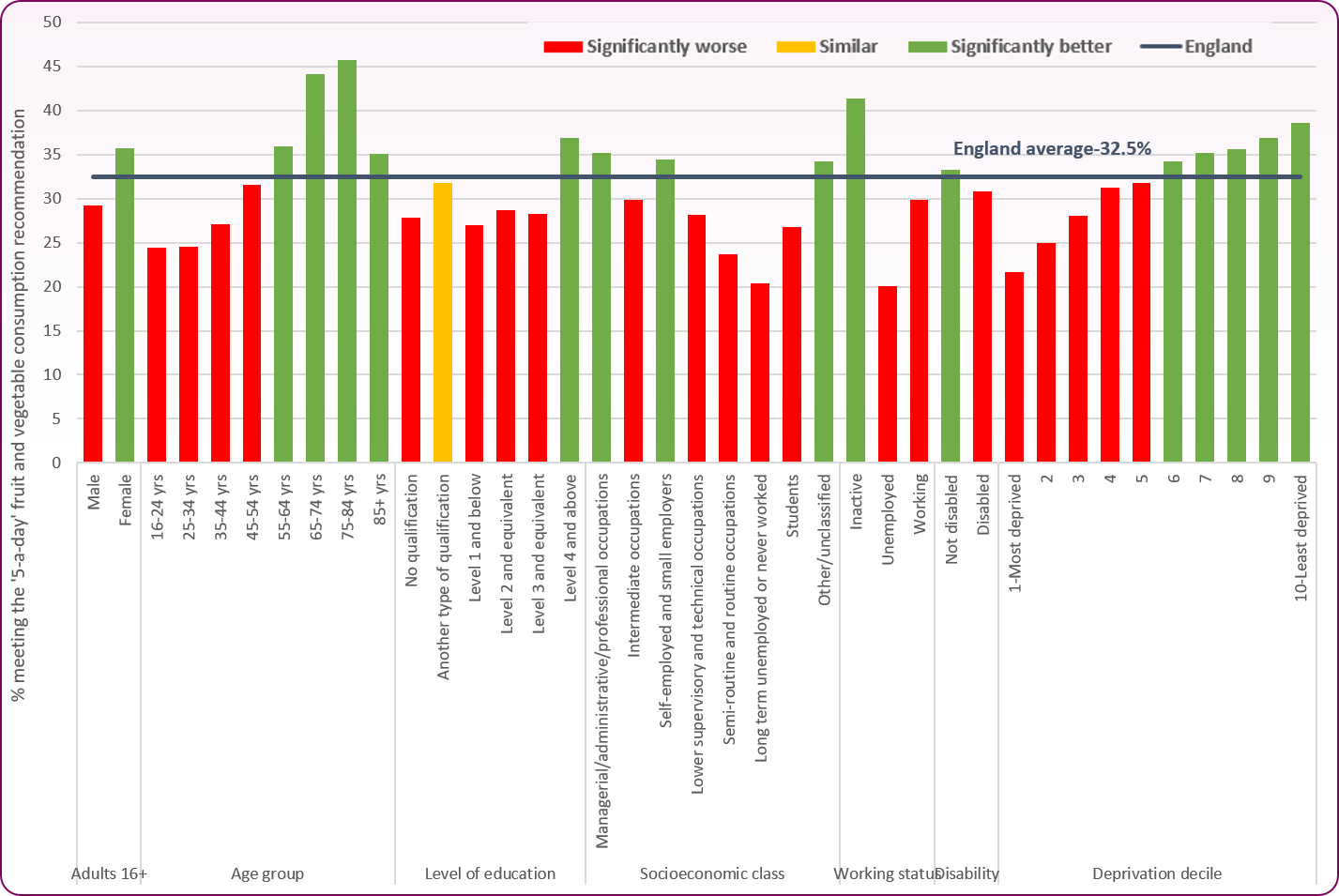 Source: OHID, Obesity Profile
Source: OHID, Obesity Profile
Income is not the only factor which can influence healthy eating; cooking and storage facilities or the cost of gas/electricity can be problematic for some, as can a lack of knowledge around food preparation. In these situations convenience foods are more likely to be eaten - this includes processed foods and takeaway/fast food. Data from the Blackpool Lifestyle Survey in 2015 shows:
-
- 20% reported eating fast food or takeaway meals at least once a week
- Almost 10% said they never prepared a meal from basic ingredients
- A further 14% said they prepared a meal from basic ingredients less than once a week
- Younger people (age <45) eat takeaway food more often than older people and those working full time eat takeaway food significantly more frequently
- Those not in work are significantly less likely to prepare a meal from scratch
Soft and fizzy drinks can be high in sugar (which can damage children's teeth) and have few nutrients. Children and adults who have a lot of sugary soft and fizzy drinks are more likely to put on weight and to be overweight or obese.
- 14% of people reported consuming fizzy drinks 6 or more times a week
- People who are obese are significantly more likely to consume fizzy drinks more often
- The number of fizzy drinks consumed decreases with age and financial security
Risk factors
The benefits of maintaining a healthy weight and nutrition are numerous, not only to the quality of life, but also the quantity of life. An unhealthy body weight is a burden and can lead to an individual being overweight or obese. If you are overweight or obese, you have a higher risk of developing serious health problems , as well as having an impact on the wider society and the economy.
Key research shows that households/individuals who are in poverty or socially disadvantaged have worse dietary-related outcomes. Those who are most likely to experience food poverty are6:
-
- people living on low incomes or who are unemployed
- households with dependent children
- older people
- people with disabilities
- members of black and minority ethnic communities
National and local guidance
Blackpool’s Healthy Weight Strategy 2023-2028 details the town’s obesity issues, provides information about why action is required and explores how different stakeholders and partners can contribute to tackling this agenda. This strategy sets out Blackpool’s five year vision, ambition and priorities.
Better Health-Healthier Families (previously Change4Life) is an NHS initiative which provides information and advice on eating, drinking and leading a more active life.
School Food Standards (2015). A new set of standards for food provided in schools is now mandatory in all maintained schools and new academies and free schools, from January 2015. The standards aim to help children develop healthy eating habits and ensure they get the energy and nutrition they need across the whole school day
PHE have produced an evidence review of measures to reduce sugar consumption, October 2015
NICE Quality standard 94: Obesity prevention and lifestyles weight managements in children and young people; July 2015 - This guidance covers a fanve of approaches at a population level to prevent children and young people aged under 18 from becoming overweight or obese. It includes interventions for lifestyle weight management
NICE Guidance 7: and preventing excess weight gain amongst adults and children; March 2015
OHID, Healthy eating: applying All Our Health, January 2023. Part of ‘All Our Health’, the information in this module is aimed at the general population and will help frontline staff promote the benefits of a healthy, balanced diet.
Recommendations
The ambition of Blackpool's Healthy Weight Strategy 2023-28 is to ensure the population of Blackpool and future generations have the best start in life, live longer and happier lives. The aim is to encourage making a healthier choice the easy choice and for individuals to feel enabled to make positive lifestyle choices to sustain or maintain a healthy weight by working together with a range of partners and sectors to make changes to our food, physical activity and social environment to promote healthy weight.
Blackpool Priorities
-
- Supporting our children and young people develop, grow and to be a healthy weight
- Promoting Healthier food and exercise choices across the town
- Help to provide food security for all Blackpool residents and enable them to manage and prepare food to provide nutritious meals cost effectively
- Ensuring people have access to the right information and resources to make healthy choices that support effective weight management
- Promote and support active lifestyles, encourage the population to move more including the use of public transport, cycling, and walking
- Building Healthier workplaces which support employees to move more, and to make healthier choices including active travel to support employees making healthier choices
[] WHO, Healthy diet fact sheet No 394, April 2020
[] The Food Foundation, The Broken Plate: The State of the Nation's Food System, 2023
[] Persistent poverty in the UK and EU, ONS, 2017
[] OHID, Obesity Profile, October 2023
[] OHID, National General Practice Profile, 2021/22
Dept for Environment, Food and Rural Affairs, UK Food Security Report 2021: Theme 4: Food Security at Household Level, October 2023