Health Care Associated Infection (HCAI)
Last Modified 09/12/2025 11:02:11
Share this page
Health Care Associated Infections (HCAI) are infections resulting from medical care or treatments in a hospital setting, primary care setting, nursing home, or the patient's own home - this definition of HCAI reflects the fact that healthcare has changed and is now often performed outside a hospital environment. HCAI's can affect any part of the body but in the UK, the gastrointestinal and respiratory systems and the urinary tract are most commonly affected.
HCAI covers a wide range of infections. The most well known include those caused by Meticillin-resistant Staphylococcus aureus (MRSA), Meticillin-sensitive Staphylococcus aureus (MSSA), Clostrididiodes difficile (C.diff) and Escherichia coli (E coli).
HCAIs potentially pose a risk to patients, clients and staff arising from treatment and care in hospital and primary care settings. They can incur significant costs for the NHS and others, and cause significant morbidity and mortality for those infected. As a result, Infection Prevention and Control is a key priority for the NHS, and Public Health England (PHE) has a responsibility to advise and support the NHS and others in their efforts to prevent HCAIs and any associated risks to health.
For Clinical Commissioning Groups (CCG) there is an expectation to continually increase standards of infection control to limit the incidence of HCAI, with the overall aim of eradicating them completely. A zero tolerance approach to MRSA and a significant reduction of reported C.difficile are linked to better patient outcomes (or a lack of harmful outcome).
PHEs annual epidemiological commentary on HCAIs for 2019 to 2020 reports that overall rates for both MRSA and C. difficile infections continue to see year-on-year reductions, though with some annual increases in more recent years. In 2019/20, 814 cases of MRSA were reported by NHS Acute Trusts in England, a decrease of 81.7% from 2007/08. The rate of cases per 100,000 population per year has fallen from 8.6 in 2007/08 to 1.5 in 2019/20. For C. difficile, a total of 13,177 cases were reported by NHS trusts in England in 2019/20, an increase of 7.4% from 2018/19, but a decrease of 76.3% from 2007/08. The overall case rate of C. difficile cases per 100,000 population per year has fallen from 107.6 in 2007/08 to 23.5 in 2019/201.
Recent declines in national rates for both MRSA and C.difficile were in both community and hospital settings, though reductions have been steeper in hospital settings.
National rates for MSSA bacteraemia and E. coli have increased year-on-year, with community-onset accounting for an increasing proportion of overall cases. The national rate of total E.coli cases per 100,000 population has risen from 60.4 in 20012/13 to 77.3 in 2019/20, though the 2019/20 rate is broadly similar to 2018/19. The national rate for all MSSA cases per 100,000 population has risen from 16.4 in 2011/12 to 21.8 in 2019/20, with an increase of 0.8% between 2018/19 and 2019/201.
The report estimates that a large proportion of community-onset infections had recent healthcare interactions, and if significant reductions in cases are to be achieved it will be important to focus on community interventions and improving infection control at the interface between hospital and community.
Public Health England data shows that:
- In 2019/20, Blackpool hospitals had only 5 reported cases of MRSA (bloodstream infection), a rate of 2.3 per 100,000 bed days. This compares with 2.4 per 100,000 bed days nationally. In 2020/21 there were also 5 reported cases at a rate of 2.6 per 100,000 bed days (compared to 2.4 per 100,000 bed days nationally).
- In 2019/20, Blackpool CCG2 saw a rise in the rate of MRSA infection from around 1.4 per 100,000 population during 2018/19 to 3.6 per 100,000 (based on 12-month rolling average, March 2020). The 2020/21 rate was 2.9 per 100,000, compared to an England average of 1.2.
- There were 186 cases of C. difficile reported by Blackpool hospitals in 2019/20, a rate of 85 per 100,000 bed days compared to 38.1 nationally. For 2021/22 this rate fell to 71.5 per 100,000 bed days (compared to a rate of 45.3 nationally), with 140 reported cases.
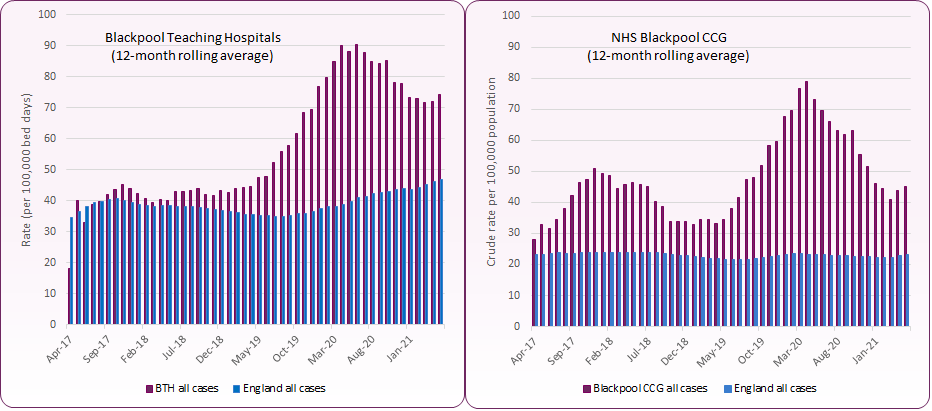
Figure 1 shows the trend in rates of C. difficile infection at hospital and CCG levels2. Cases in Blackpool rose from late 2018 to the middle of 2020 when they began to fall across both the hospital and CCG. Rates in the CCG rose from 33 per 100,000 population in January 2019 to a peak of 79 per 100,000 by April 2020, before falling back to 45.2 per 100,000 by March 2021 (based on a 12-month rolling average) . This remains significantly higher than the national average of 23.1 per 100,000, and is the second highest rate in the country behind NHS Fylde &Wyre CCG.
Blackpool Teaching Hospitals NHS Trust has seen a similar rise, going from a rate of 41.7 per 100,000 bed days in November 2018 to 90.5 per 100,000 by June 2020, before falling to 74.1 per 100,000 bed days by March 2021 (based on a 12-month rolling average). As the chart shows, this rate remains significantly higher than England average of 46.7 (May 2021).
Figure 1: Trend in rates of C.difficile - Blackpool Teaching Hospitals, Blackpool CCG and England average
 Source: PHE, Public Health Profiles, Clostrididiodes difficile infection.
Source: PHE, Public Health Profiles, Clostrididiodes difficile infection.
From April 2017 Public Health England introduced a new categorisation system to aid the identification of the origin of C. difficile cases and the apportionment of cases between healthcare and community settings. On the basis of the timing of detection of the virus and prior history of hospital admission, C. difficile cases are categorised in the following ways:
- Healthcare / Hospital Onset - Healthcare Associated (HOHA): onset between 2 days after admission up to point of discharge
- Community Onset - Healthcare Associated (COHA): onset up to 4 weeks after hospital discharge
- Community Onset - Intermediate Association (COIA): onset between 4 and 8 weeks after hospital discharge
- Community Onset - Community Associated (COCA): onset 8 weeks and beyond discharge
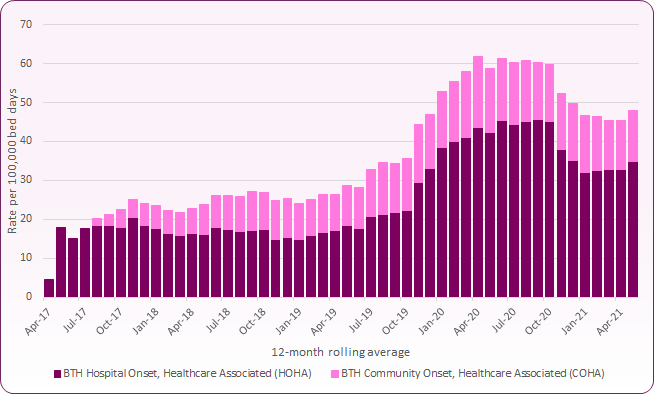
For Blackpool Teaching Hospitals Acute NHS Trust, the 2018/19 crude rate of Hospital Onset Healthcare Associated (HOHA) C. difficile infections was 16.6 per 100,000 bed-days, slightly higher than 15.8 the previous year. This compares to a 2018/19 England average rate of 14.1 per 100,000 bed-days. The 2018/19 rate for Community Onset Healthcare Associated C.difficile was 9.6 per 100,000 bed-days, compared to 6.6 nationally. Figure 2 shows hospital onset and community onset healthcare associated C. difficile cases for Blackpool Teaching Hopsitals as a 12-month rolling crude rate to May 2021.
Figure 2: Hospital and Community Onset Healthcare Associated C. Difficile, Blackpool Teaching Hospitals NHS Trust, April 2017 to May 2021 (12-month rolling average, crude rate per 100,000 bed days)
 Source: PHE, Public Health Profiles, Clostrididiodes difficile infection.
Source: PHE, Public Health Profiles, Clostrididiodes difficile infection.
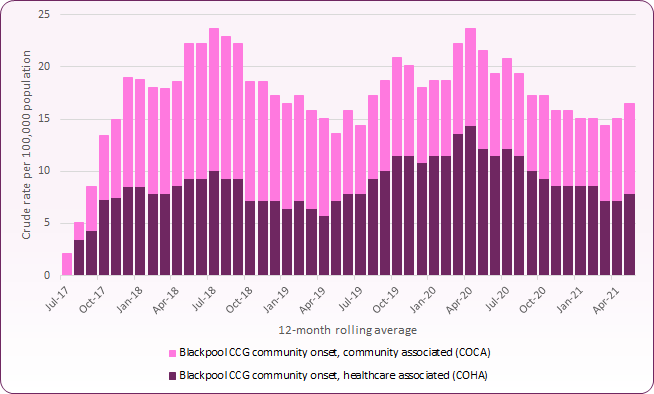
Similarly, PHE reports rates for Blackpool CCG for Community Onset - Healthcare Associated (COHA) and Community Onset - Community Associated (COCA) C. difficile based on a crude rate per 100,000 population (Figure 3). Rolling 12-month rates for COCA C.difficile have remained relatively stable in recent years (7.9 per 100,000 population at March 2021 compared to the national average of 7.1). However, community onset, healthcare associated rates have fluctuated, peaking at 14.4 per 100,00 population in April 2020 before falling to 7.9 per 100,000 in May 2021. This is significantly higher than the England rate of 4.1.
Figure 2: Community Onset C. Difficile Rates, Blackpool CCG, April 2017 to May 2021 (12-month rolling average, crude rate per 100,000 population)
National and local guidance
PHE provides HCAI guidance, data and analysis which monitors the numbers of certain infections that occur in healthcare settings through routine surveillance programmes, and advises on how to prevent and control infection in establishments such as hospitals, care homes and schools.
NICE guideline [NG199] Clostridioides difficile infection: antimicrobial prescribing (July 2021) sets out an antimicrobial prescribing strategy for managing Clostridioides difficile infection in adults, young people and children aged 72 hours and over in community and hospital settings.
HCAI Operational guidance (2013) provides the steps health protection teams will need to take to make sure they meet healthcare associated infections (HCAIs) standards.
The Health and Social Care Act 2008: code of practice on the prevention and control of infections and related guidance.
PHE gives information on antimicrobial resistance (AMR), sets out effective methods to avoid unnecessary prescribing of antibiotics and provides advice for healthcare professionals.
Risk factors
Several factors can cause health care-associated infections3. Some of these factors are present regardless of the resources available:
-
- prolonged and inappropriate use of invasive devices and antibiotics,
- high-risk and sophisticated procedures,
- immuno-suppression and other severe underlying patient conditions,
- insufficient application of standard and isolation precautions.
Some determinants are more specific to settings with limited resources:
-
- inadequate environmental hygienic conditions and waste disposal,
- poor infrastructure,
- insufficient equipment,
- understaffing,
- overcrowding,
- poor knowledge and application of basic infection control measures,
- lack of procedure,
- lack of knowledge of injection and blood transfusion safety,
- absence of local and national guidelines and policies.
Antibiotic consumption in England is on the rise and increased antibiotic prescribing is fuelling increased resistance in bacteria. PHE wants to see a reduction in the number of infections caused by antibiotic resistant bacteria4. Antibiotic prescribing and antibiotic resistance are inextricably linked and areas with high levels of antibiotic prescribing also have high levels of resistance.
[] PHE, Annual Epidemiological Commentary: Gram-negative bacteraemia, MRSA bacteraemia, MSSA bacteraemia and C. difficile infections, up to and including financial year April 2019 to March 2020.
[] Apportioned cases are assigned to the hospital or CCG when the Post Infection Review (PIR) indicates which organisation is best placed to ensure any lessons learned are actioned.
[] WHO, Health care associated infections fact sheet, 2011
[] PHE, Health matters: antimicrobial resistance, December 2015