Blood-borne viruses (BBV)
Last Modified 09/12/2025 11:15:20
Share this page
Introduction
Blood-borne viruses (BBVs) are viruses that some people carry in their blood and can be spread from one person to another. Those infected with a BBV may show little or no symptoms of serious disease, but other infected people may be severely ill. You can become infected with a virus whether the person who infects you appears to be ill or not - indeed, they may be unaware they are ill as some persistent viral infections do not cause symptoms. An infected person can transmit blood-borne viruses from one person to another by various routes and over a prolonged time period.
The most prevalent BBVs are:
-
- human immunodeficiency virus (HIV) - a virus which causes acquired immunodeficiency virus (AIDS), a disease affecting the body's immune system;
- hepatitis B (HBV) and hepatitis C (HCV); BBVs causing hepatitis, a disease affecting the liver. (There are also further types of hepatitis spread by other means)
Facts, figures and trends
The UK falls into the lowest category of prevalence for Hepatitis B, as determined by the World Health Organisation (the prevalence rate is believed to be between 0.1% and 0.5% of the UK population) but liver disease is one of the top causes of death in England and people are dying from it at younger ages. Most liver disease is preventable and much is influenced by the prevalence of hepatitis B and hepatitis C infections, which are both amenable to public health interventions1.
Hepatitis B
Hepatitis B is transmitted by parenteral (subcutaneous, intramuscular or intravenous) exposure to infected blood and body fluids containing blood, including sexual contact, blood-to-blood contact and perinatal transmission from mother to child. The hepatitis B virus (HBV) can be prevented by immunisation, and in the UK immunisation is recommended for individuals at increased risk of exposure (see 'Risk Factors' and 'Prevention' below). In August 2017, HPV vaccination was also introduced into the UK's routine infant immunisation programme.
A total of 381 acute or probable acute cases of hepatitis B were reported for England in 2018, an annual incidence rate of 0.68 per 100,000 population. The North West rate was 0.62 per 100,000 for this period. Rates for both England and the North West region show a general downward trend over the past ten years (Figure 1). The incidence rate for Blackpool for both 2017 and 2018 has remained stable at 0.71 per 100,000 population, however very low case numbers mean that local rates cannot be reported with confidence.
Figure 1: Trend in incidence of acute/probable acute hepatitis B, England and the North West
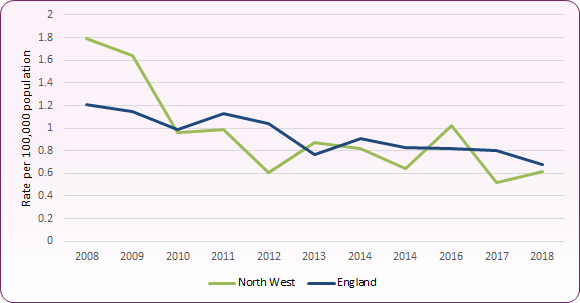 Source: PHE, Health Protection Report, Acute hepatitis B (England): annual reports for 2014 and 2018
Source: PHE, Health Protection Report, Acute hepatitis B (England): annual reports for 2014 and 2018
Hepatitis C
The hepatitis C virus (HCV) infects and damages the liver, with persistent infection leading to cirrhosis, liver failure or cancer. Since most HCV infections are asymptomatic for years people are often unaware of their infection until the liver becomes severely damaged. The virus is particularly concentrated in the blood of an infected person, so it is usually transmitted through blood-to-blood contact, for example by sharing razors, toothbrushes or unsterilised needles (for example while injecting drugs), though it can also be transmitted from mother to her baby during pregnancy or childbirth and through sex, though this is rare2,3. Chronic hepatitis C is treatable, and direct acting antivirals tablets (DAAs) are effective in clearing the infection in more than 90% of people. Treatment does not, however, prevent reinfection.
In May 2016 the World Health Organisation adopted a Global Health Sector Strategy on viral hepatitis, introducing a target of 30% reduction in new cases of hepatitis B and C by 2020 and a 10% reduction in mortality. In the UK in 2017 around 118,000 individuals were estimated to have long-term (chronic) infection with hepatitis C, a reduction from around 174,000 in 20152. 26,750 people are estimated to be living with chronic HCV in the North West, with around 8,500 of these living across Lancashire and Cumbria4.
Injecting drug use is the largest risk factor for HCV infection in the UK, with more than 90% of laboratory reports where risk factors are disclosed citing injecting drug use as the individual's HCV risk. Data from the Unlinked Anonymous Monitoring (UAM) survey of people who inject drugs (PWID) in 2019 suggests that just over half (54%) of this group had evidence of ever being infected with HCV, and just less than a quarter (23%) had evidence of current infection. Whilst data for England shows a reduction in the overall prevalence of chronic HCV infection, chronic infection remains stable in those who are injecting drugs.
Figure 2: Trend in anti-HCV prevalence among people who inject drugs in England: 2010-2019 (UAM Survey)
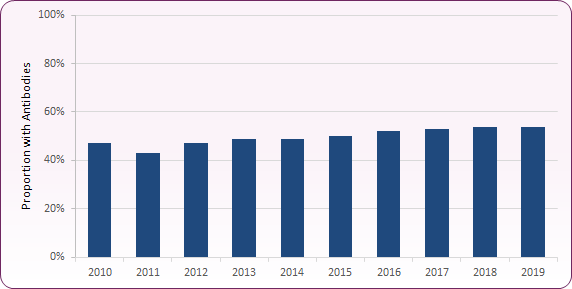 Source: PHE, People who inject drugs: HIV and viral hepatitis unlinked anonymous monitoring survey tables (psychoactive): 2021 update
Source: PHE, People who inject drugs: HIV and viral hepatitis unlinked anonymous monitoring survey tables (psychoactive): 2021 update
There is limited local data on Hepatitis B and C in Blackpool but information from Public Health England shows that:-
-
- Of the people in substance misuse treatment who inject drugs, 90.3% have received the hepatitis C test compared to 84.2% nationally
- Under 75 mortality from hepatitis C related end-stage liver disease/hepatocellular carcinoma (1.58 per 100,000) is significantly higher than the national average (0.53)
- The 2017 hepatitis C detection rate (the rate of new diagnoses per 100,000 population) in Blackpool was 57.1, over three times the national average of 18.4. This increased from a rate of 19.7 in 2016.
Figure 3: Blackpool health indicators relating to hepatitis from Public Health England Profiles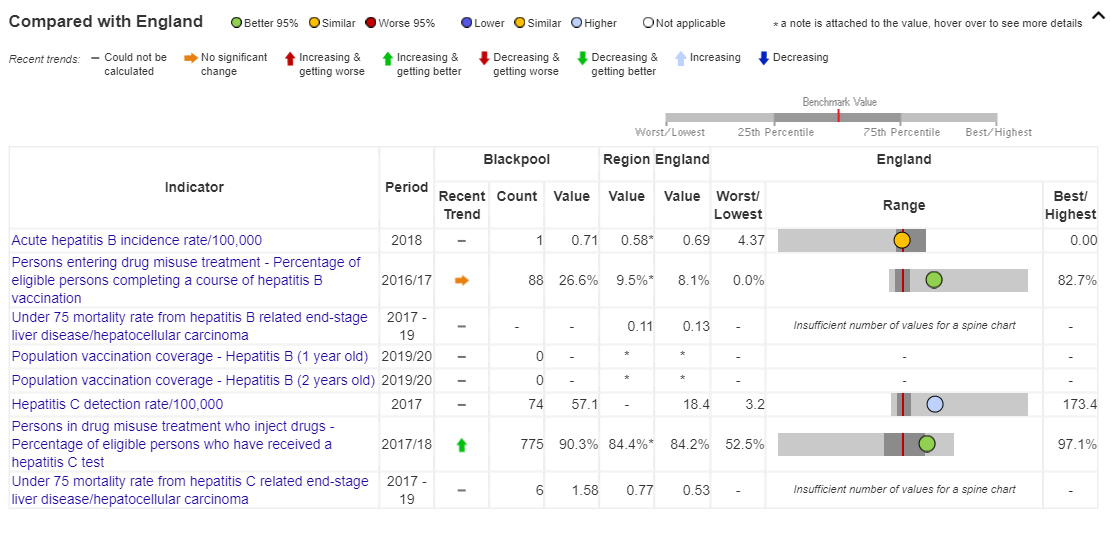 Source: Public Health England Profiles, December 2021
Source: Public Health England Profiles, December 2021
Information on human immunodeficiency virus (HIV) can be found in the HIV/AIDS section
National and local guidance
Preventing the spread of blood-borne viruses (BBVs) is a key public health issue, and a key outcome in the UK Government Drug Strategy 2010 and Drug Strategy 2017.
Hepatitis C: guidance, data and analysis provides information on the characteristics, diagnosis, management and epidemiology of hepatitis C (Hep C, HCV).
Hepatitis B: guidance, data and analysis provides information on the characteristics, diagnosis, management and epidemiology of hepatitis B
Risk factors
Throughout the UK, injecting drug use continues to be the most important risk factor for hepatitis C infection therefore monitoring infection among this important risk group remains a UK priority.
Hepatitis B infection is by exposure to infected blood and body fluids, most often through sexual contact, blood to-blood contact and perinatal transmission from mother to child. HBV infection can be prevented by vaccination and in the UK immunisation is used for individuals at high risk of exposure to the virus e.g. people who inject drugs (PWID), healthcare workers. Immediate post-exposure vaccination is used to prevent infection, especially in babies born to infected mothers or following needle-stick injuries.
Prevention
Ensuring people who use drugs do not contract BBVs is one way of keeping them and their communities' safe before and during their recovery journeys. Preventing BBV transmission also has benefits for wider society, both in terms of reducing health harms, and reduced treatment costs. Effective local action to prevent BBVs will include a range of services. BBV transmission can be prevented by:
-
- Needle and syringe programmes: pharmacy, specialist, outreach/mobile, in hostels and gyms
- Comprehensive protocols to raise awareness of risks from BBVs which promote and deliver testing and appropriate pathways into treatment for hepatitis B, hepatitis C and HIV, and vaccination against hepatitis B
- Provision of advice and materials to reduce harm from injecting drug use
- Offers of testing and/or vaccination to all those at risk of contracting BBVs
- Programmes that prevent the uptake of injecting drug use and promote switching from injecting drug use to other means of administration
- Workforce and occupational health interventions for people working with those at risk of contracting BBVs
Vaccination against Hepatitis B would usually only be recommended for people in high-risk groups, such as:
-
- people who inject drugs or have a sexual partner who injects drugs
- people who change their sexual partner frequently
- people travelling to or from a part of the world where hepatitis B is widespread
- healthcare workers who may have come into contact with the virus
[1] PHE, Acute Hepatitis B (England): annual report for 2018
[2] PHE, Hepatitis C in the UK, 2020
[3] NHS England Hepatitis C Factsheet.
[4] PHE, Hepatitis C in the North West, 2017 data