Children and Young People's Mental Health: Rapid Needs Assessment
Last Modified 17/12/2025 13:36:26
Share this page
Mental health can impact on all areas of young people's lives - how they feel about themselves and others, their relationships and their psychological and emotional development. Poor mental health underlies many risk behaviours, including smoking, alcohol and drug misuse and higher-risk sexual behaviour.1 Being mentally healthy helps people to realise their potential, gives them strength to cope with change, overcome challenges and adversity, and make a positive contribution to their community.2
One in nine (11.6%) children and young people aged between 6 and 16 years had at least one probable mental disorder when surveyed in 2017. In 2023 this was one in five 8 to 16-year-olds (20.3%). After a rise in prevalence between 2017 and 2020, rates of probable mental disorder remained stable in all age groups (8 to 25-years) between 2022 and 2023.3,4 For some, mental health issues may resolve with time, though many continue to have difficulties into adulthood.
A 2021 study found that the peak age of onset of mental health conditions worldwide was 14.5 years.5 Half of those with lifetime mental health conditions first experience symptoms by the age of 14, and three-quarters before their mid-20s.6,7
Mental health conditions can be grouped into four types:
- Emotional disorders - e.g. anxiety disorders, depressive disorders, mania and bipolar affective disorder. One in 12 (8.1%) of 5 to 19 year olds had an emotional disorder in 2017, with rates higher in girls (10%) than boys (6.2%).
- Behavioural (or conduct) disorders - repetitive and persistent patterns of disruptive and violent behaviour. About one in twenty (4.6%) 5-19s had a behavioural disorder, with rates higher in boys (5.8%) than girls (3.4%).
- Hyperactivity disorders - characterised by inattention, impulsivity and hyperactivity. About one in sixty (1.6%) 5-19s had a hyperactivity disorder, with rates higher in boys (2.6%) than girls (0.6%).
- Other less common disorders - e.g. autistic spectrum disorders, eating disorders and tic disorders. About one in fifty 5-19s were identified with one or more of these types of disorder.3
Conditions most frequently experienced in adolescence include anxiety and depression, behavioural disorders, eating disorders, and self-harm. Many of these conditions are preventable and good mental health promotion and early intervention can mean that children and young people get the right support at the right time to prevent them reaching crisis point.8
A range of factors impact on a child's mental health and wellbeing, ranging from genetic influences and disability to educational difficulties, bullying, problems with friendships, family problems, socio-economic disadvantage, inequalities and other 'adverse childhood experiences' including abuse, neglect, bereavement, parental substance misuse or domestic violence.8,9
With high levels of poverty, deprivation and rates of children in need or who are looked after, a relatively high proportion of children and young people in Blackpool are likely to face challenges that impact negatively on their mental health and wellbeing. For additional information about how these impact on Blackpool see the 2019 Children and Young People's Mental Health: Rapid Needs Assessment  (1.33 MB).
(1.33 MB).
Estimated national prevalence of mental health conditions in children and young people
The NHS Digital Mental Health of Children and Young People Survey in England was carried out in 1999, 2004, and 2017.3 The 2017 survey collected information about 9,117 children and young people across the country between January and October 2017, with 4,000 of these aged 11-19. Young people and their carers completed standardised tools that measured disorders as specified in the International Classification of Disease (ICD-10) diagnostic criteria. Findings showed that:
-
- One in eight (12.8%) 5 to 19-year-olds had at least one probable mental disorder when assessed in 2017;
- Emotional disorders were the most prevalent type of disorder experienced by 5 to 19-year-olds in 2017 (8.1%). Higher rates were found in girls (10.0%) than boys (6.2%). Anxiety disorders (7.2%) were more common than depressive disorders (2.1%).
- Rates of mental disorders increased with age. 5.5% of 2 to 4-year-old children experienced a mental disorder, compared to 16.9% of 17 to 19-year-olds. Caution is needed, however, when comparing rates between age groups due to differences in data collection.
- Data from this survey series reveal a slight increase over time in the overall prevalence of mental disorder in 5 to 15-year-olds (the age group covered on all surveys in this series). Rising from 9.7% in 1999 and 10.1% in 2004, to 11.2% in 2017.
- Emotional disorders have become more common in 5 to 15-year-olds - going from 4.3% in 1999 and 3.9% in 2004 to 5.8% in 2017. This increase was evident in both males and females.
- All other types of disorder, such as behavioural, hyperactivity and other less common disorders, have remained similar in prevalence for this age group since 1999. Conduct disorder was higher in boys (5.8%) than girls (3.4%), as was hyperactivity disorder (2.6% for boys, compared to 0.6% for girls).
Follow-up surveys were conducted in 2020 (wave 1), 2021 (wave 2), 2022 (wave 3), and 2023 (wave 4). The wave 4 survey questioned 2,370 children and young people from the 2017 survey.4 It focused on 8 to 25-year-olds' household circumstances, family life, and experiences of education and services. Where possible, comparisons are made to earlier surveys. Findings for 2023 (wave 4) show:
-
- Rates of probable mental disorder (PMD) increased from 11.6% (for 6 to 16-year-olds) in 2017 to 20.3% in 8 to 16-year-olds, 23.3% in 17 to 19-year-olds, and 21.7% in 20 to 25-year-olds. After a rise in prevalence between 2017 and 2020, rates of PMD remained stable between 2022 and 2023.
-
Rates of PMD are similar for boys and girls aged 8 to 16-years. For 17 to 25-year-olds, rates are double for females, compared to males.
-
The proportion of children and young people aged 11 to 16 with eating disorders increased to 12.3% from 6.7% in 2017. For those aged 17 to 19 it increased from 44.6% in 2017 to 59.4%.
-
39.1% of 8 to 16-year-olds and 64.9% of 17 to 23-year-olds had sleep problems on three or more nights of the previous week. In 2021 this was 33.0% of 6 to 16-year-olds, and 57.1% of 17 to 23-year-olds.
-
Children and young people with any PMD are more likely to have sleep problems (76.5% for those aged 8 to 16 and 91.4% for 17 to 23-year-olds).
-
3.8% of 8 to 16-year-olds missed more than 15 days of school (based on the 2022 autumn term). This is a reduction from 10.6% of 6 to 16-year-olds who missed more than 15 days of school during the 2020 autumn term (during the COVID-19 period). Those with a PMD are three times more likely to have missed 15 days or more (13.4% compared to 4.1% of those unlikely to have a mental disorder).
-
Children aged 11 to 16 with a PMD are five times more likely to have been bullied than those who are unlikely to have a mental disorder (36.9% and 7.6% respectively).
- 18.7% of 8 to 16-year-olds with a PMD live in households that had fallen behind with bills, rent or mortgage and 15.3% could not afford to buy enough food, or had to use a food bank. For those unlikely to have a mental disorder the figures are 6.8% and 3.5% respectively. In 2021 the figures were 12.8% (fallen behind with bills) and 9.1% (couldn’t afford food) for those with a PMD.
Children and young people's mental wellbeing in Blackpool
In Blackpool, the council's Health Related Behaviour Survey collects information about the health and lifestyles of young people aged 8 to 11 and 12 to 15 every two years. In the 2019 survey a total of 1,889 pupils took part across 19 primary and three secondary schools. The survey does not explore mental health conditions, but explores wider issues of mental wellbeing. In 2019:
-
- For those aged 8-11 years:
- 28% of boys and 25% of girls had high self-esteem scores. This compares to 30% boys and 26% girls in 2017, and 37% boys and 25% girls in 2015.
- 9% had low self-esteem scores (7% in 2017, 9% in 2015).
- 61% of Year 6 girls worried about SATs / tests, 37% about problems with friends, 34% about family, 31% about the way they looked and 24% about crime.
- 41% of Year 6 boys worried about SATS / tests, 33% about family, 30% about crime, 22% about problems with friends, and 19% about health.
- 30% of pupils reported that they had been bullied at or near school in the last 12 months (23% in 2017, 21% in 2015).
- For those aged 12-15 years:
- 42% of boys and 20% of girls had high self-esteem scores. This compares to 42% and 26% in 2017, and 46% and 25% in 2015.
- 9% had low self-esteem scores (7% in 2015 and 2017).
- 61% of Year 10 girls worried about exams and tests, 52% about they way they looked, 49% their weight and 23% family problems.
- 31% of Year 10 boys worried about exams and tests, 15% about money, 14% about family problems and 14% about school work.
- 23% of pupils reported that they had been bullied at or near school in the last 12 months (22% in 2017, 25% in 2015).10
Hospital admissions for mental health conditions
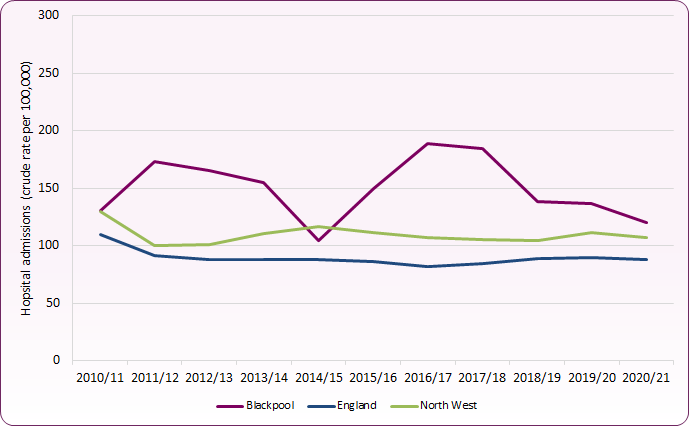
The COVID-19 period had a significant impact on hospital admissions across the country, and data for the 2020/21 period is likely to be affected by this and other effects of COVID-19 restrictions (for example, reduced presentation to, or availability of, support and referral services during lockdown periods). In 2020/21 around 35 young people were admitted to hospital with a primary diagnosis of mental and behavioural disorders - a rate of 120.2 per 100,000.
Across Blackpool in 2021/22, around 45 young people aged under-18 years were admitted to hospital with a primary diagnosis of mental and behavioural disorders - a rate of 161.8 per 100,000 population, which is significantly higher than the rate for England (99.8). Following the census in 2021, population estimates are being revised. This means direct comparisons between the 2021/22 rate and previous rates cannot be made, neither can the trend chart be updated at this stage to incorporate the 2021/22 rate (figure 1).11
Figure 1: rates of hospital admissions for mental health conditions for young people aged 0-17 (per 100,000 population)
 Source: Office for Health Improvement & Disparities Child and Maternal Health, Child Health Profiles / HSCIC Hospital Episode Statistics, 2021.
Source: Office for Health Improvement & Disparities Child and Maternal Health, Child Health Profiles / HSCIC Hospital Episode Statistics, 2021.
Self-harm
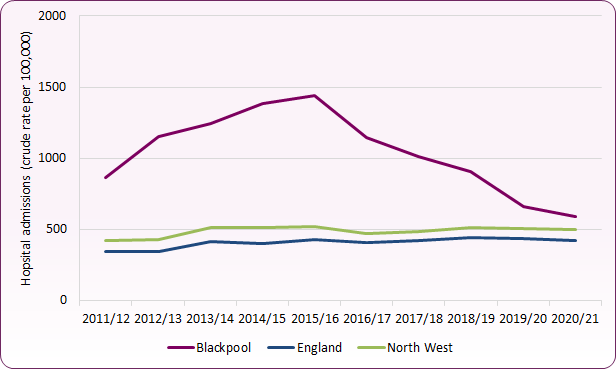
Self-harm in itself is not a psychiatric disorder but is a sign of mental distress. Engaging in self-harm can be a maladaptive coping mechanism, as a young person may use it as a way of coping with distressing feelings.12 Nationally, the rate of young people being admitted to hospital as a result of self-harm is relatively stable. The trend across Blackpool has been significantly higher than the England average for a number of years and peaked in 2015/16 with 349 admissions, a rate of 1,438 per 100,000 population (aged 10-24). Since then admissions have fallen and in 2020/21 there were around 135 admissions at a rate of 594 per 100,000, though with hospital admissions affected by COVID-19 it is not possible to determine the extent to which this reduction is due to the wider factors affecting the NHS and other services over this period (figure 2).
In 2021/22 the rate was 679.8 (per 100,000 aged 10-24), significantly higher than England (427.3), although as for the admissions for mental health conditions (above), this rate cannot be directly compared to previous years due to the population revisions from the census.
The Child & Adolescent Support & Help Enhance Response (CASHER) team may be a contributory factor in this decline in admissions. Introduced at the end of 2015, CASHER is a multidisciplinary team providing out of hours mental health support to young people under the age of 25. The CASHER team are based at Blackpool Victoria Hospital and provide weekend clinics and evening groups for young people in community venues.
Figure 2: young people aged 10 to 24-years admitted to hospital as a result of self-harm (rate per 100,000 pop.)
 Source: Office for Health Improvement & Disparities, Children and Young People's Mental Health and Wellbeing
Source: Office for Health Improvement & Disparities, Children and Young People's Mental Health and Wellbeing
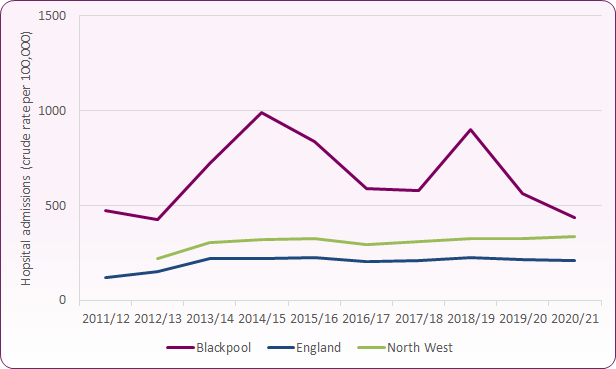
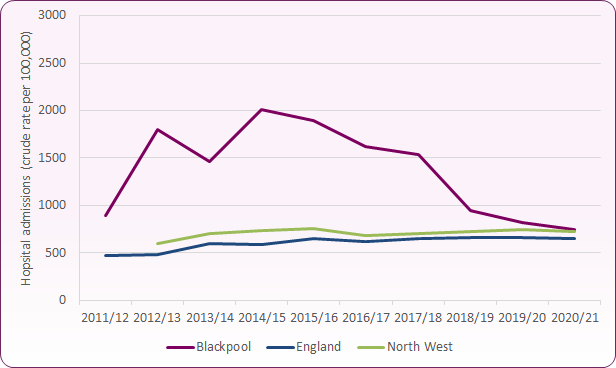
Approximately 39% of admissions for self-harm in 2019/20 were in the 15-19 age group (n=60), 32% in the 20-24 age group (50) and 29% in the 10-14 age group (45).13 Figures 3-5 below show trends in rates of admissions for these age groups for Blackpool and England. Whilst falls in hospital admissions have been observed in both 15-19 and 20-24 age groups since 2015/16, this decline is not as evident in the 10-14 age range.
Figures for COVID-19-affected 2020/21 show a decline in admissions across all age groups, though the proportion of admissions across the groups were similar. The number of admissions of 15 to 19 year old females did, however, increase slightly during this period, with approximately 50 admissions at a rate of 1,405 per 100,000, compared to around 45 (1,258 per 100,000) in 2019/20.
Figure 3: rates of hospital admissions as a result of self-harm 10-14-years (per 100,000 population)
 Source: Office for Health Improvement & Disparities, Children and Young People's Mental Health and Wellbeing
Source: Office for Health Improvement & Disparities, Children and Young People's Mental Health and Wellbeing
Figure 4: rates of hospital admissions as a result of self-harm 15-19-years (per 100,000 population)
 Source: Office for Health Improvement & Disparities, Children and Young People's Mental Health and Wellbeing
Source: Office for Health Improvement & Disparities, Children and Young People's Mental Health and Wellbeing
Figure 5: rates of hospital admissions as a result of self-harm 20-24-years (per 100,000 population)
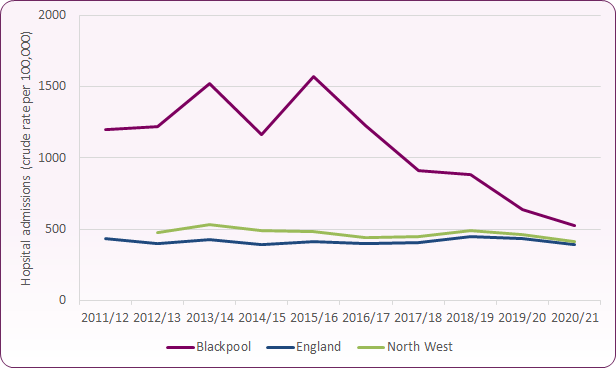 Source: Office for Health Improvement & Disparities, Children and Young People's Mental Health and Wellbeing
Source: Office for Health Improvement & Disparities, Children and Young People's Mental Health and Wellbeing
Over three-quarters of all self-harm admissions for 10-24-year-olds in Blackpool in 2019/20 and 2020/21 were for females. This is also the case nationally (77% in 2019/20 and 79% in 2020/21), a proportion that has remained relatively stable in recent years. There are, however, local gender variations across age groups: in 2019/20 approximately 89% of admissions for 10-14 year olds in Blackpool were for females, compared to 49% nationally. 75% of admissions in the 15-19 age range were female (80% nationally), and 60% of admissions in the 20-24 age range were female (68% nationally).
A local analysis of Hospital Episode Statistics data from 2015/16 to 2017/18 also showed a wide variation in admissions for self-harm across Blackpool wards. Admission rates were seven times higher in Claremont (2,587.4 per 100,000) than in Norbreck (367.9 per 100,000). Over the three-year period almost half of all hospital admissions (46%) came from Bloomfield, Claremont, Hawes Side, Park and Talbot wards.
Other sources of data also give an indication of the extent of self-harm among children and young people in Blackpool. The Blackpool Health Related Behaviour Survey (2019) found that 9% of Year 8 students who responded to the question reported having 'cut or hurt myself' when feeling stressed (5% of males and 14% of females).10 Among Year 10 students, 5% reported having 'cut or hurt myself', 4% of males and 7% of females. Overall 7% of children reported self-harm in response to stress.
In the 2017 survey, 4% of female and 4% of male respondents in Year 8 reported having 'cut or hurt myself' when feeling stressed. In Year 10 these figures increased to 6% of males and 9% of females. Overall 6% of children reported self-harm in response to stress. Relatively low numbers mean that year on year variations within subpopulations of the survey may not necessarily reflect trends, however, the overall proportion of children reporting self-harm has remained relatively stable at 6-7% (increasing slightly in 2019).
Suicide
As the 2021 NCMD report 'Suicide in Children and Young People' highlights, every death of a child or young person by suicide represents a devastating loss for families and friends, and can impact on future generations and the wider community. In 2019/20 the rate of suicide among 9 to 17 year olds in England was 1.8 per 100,000, with 108 deaths assessed as highly or moderately likely to be due to suicide. 61% of deaths were among males (a rate of 2.2 per 100,000), and 78% among those aged between 15 and 17 years.14
Between 2019 and 2021 there were a total of 67 suicides (aged 10 and over) in Blackpool, a rate of 18.7 per 100,000 population, compared to 10.4 across England. As is the case nationally, deaths from suicide are just over three times more common among males: 28.2 per 100,000 compared to 9.7 per 100,000 for females. A small proportion of suicides in Blackpool were among young people aged under-25 (numbers and proportion withheld to protect confidentiality and anonymity).15
A 2017 National Confidential Inquiry examined suicide by children and young people aged under 25.16 The main findings were:
-
- The number of suicides increased steadily in the late teens and early 20s. 76% of those who died were male and the male to female difference was greater in those over 20.
- Academic pressures and bullying were more common before suicide in under-20s, while workplace, housing and financial problems occurred more often in 20-24-year-olds.
- Bereavement was common in both age groups and suicide bereavement, i.e. the death of a family member or friend, was more common in the under-20s.
- 9% of under-20s who died had been looked after children. They had high rates of housing problems and suicidal ideas. Almost all had recent contact with at least one service but a third were not in recent contact with mental health care.
- 6% of under-20s and 3% of 20-24 year olds were reported to be lesbian, gay, bisexual, or transgender (LGB&T) or uncertain of their sexuality. A quarter of LGB&T under-20s had been bullied; most had previously self-harmed.
- Self-harm was reported in 52% of under-20s and 41% of 20-24 year olds who died, equivalent to around 200 deaths per year.
A more recent but smaller analysis of suicides among children and young people in 2019/20 by the National Child Mortality Database found that:14
-
- Rates of child / youth suicide were similar across all areas, including rural and urban environments, and deprived and affluent neighbourhoods.
- 62% of those cases reviewed had suffered a significant personal loss in their life prior to their death, including bereavement, and "living losses" such as loss of friendships and routine due to moving home or school or other close relationship breakdown.
- Almost a quarter of children and young people reviewed had experienced bullying either face to face or cyber bullying.
- 16% had a confirmed diagnosis of a neurodevelopmental condition at the time of their death (for example, autistic spectrum disorder and attention deficit hyperactivity disorder).
The COVID-19 period has impacted on both the wellbeing of the population and upon a wide range of health, social and other support services. Because of the effects on areas such as hospital admissions and the accessibility of services during the pandemic, it can be difficult to fully understand the impact on people's health. For example, reduced admissions for certain conditions may not be an indication of reduced need.
As reported above, NHS Digital's follow-up survey of 'Mental Health of Children and Young People in England, 2021' found that rates of probable mental disorder among 6 to 23 year olds increased between 2017 and 2021, though they remained similar between July 2020 and February / March 2021. 13.5% of 11 to 16-year-olds and 23.9% of 17 to 23-year-olds felt their lives had been made 'much worse' by coronavirus restrictions. 26.2% of the parents of 6 to 16-year-olds with a probable mental health disorder had not sought help or advice for their child between summer 2020 and spring 2021, whilst 41.5% of 17 to 23-year-olds with a probable mental health disorder had not sought help during this period.4
OHID's 'Wider Impacts of COVID-19 on Health (WICH) Monitoring Tool' explores the indirect effects of the COVID-19 pandemic on population health and wellbeing. Drawing on Office for National Statistics (ONS) Opinions and Lifestyle Survey (OPN) data, findings for the 16 to 24-year-old group show that reported low levels of life satistfaction and self-worth increased considerably during the pandemic, as did reported levels of high anxiety. Whilst all age ranges had increased proportions with reported poorer mental health / wellbeing during the pandemic, the proportion of those with low satisfaction / worth and high anxiety were regularly highest among the 16-24 group during this period, particularly during lockdown 3.17 Under-16s were not part of this survey.
In relation to suicide among children and young people, national studies by the NCMD concluded that there was no consistent evidence that child suicide deaths increased during the COVID-19 pandemic period to the end of December 2020, though it was possible that there was a higher rate during the first lockdown period compared to the corresponding period in the previous year.18
At a local level, the full impact of the COVID-19 pandemic on the mental health of children and young people in Blackpool may currently be difficult to measure, and may become more apparent as health, social and education services continue to recover and the level and extent of need becomes apparent throughout the system.
As part of the mental health services transformation work happening across Lancashire, services for children and young people's emotional health and wellbeing have been mapped against the THRIVE framework. Local statutory services have been identified in the document below. Third sector provision across Blackool has also been identified.
Royal College of Psychiatrists Position Statement PS4 (2010).
World Health Organisation (2005) Promoting Mental Health; Concepts, emerging evidence and practice.
[] NHS Digital (2018) Mental Health of Children and Young People in England, 2017.
[] NHS Digital (2023) Mental Health of Children and Young People in England, 2023: Wave 4 follow up to the 2017 survey.
[] Solmi, M., Radua, J., Olivola, M., Croce, E., Soardo, L., Salazar de Pablo, G., Shin, J., Kirkbridge, J.B., Jones, P., Kim, J.H., Kim, J.Y., Carvalho, A.F., Seeman, M.V., Correll, C.U., & Fusar-Poli, P. (2021) Age at onset of mental disorders worldwide: large-scale meta-analysis of 192 epidemiological studies. Molecular Psychiatry 2021, https://doi.org/10.1038/s41380-021-01161-7.
[] Kim-Cohen J., Caspi A., Moffitt T., Harrington, H, Milne, B.J. & Poulton, R. (2003) Prior juvenile diagnoses in adults with mental disorder. Archives of General Psychiatry 60: 709-717. doi: 10.1001/archpsyc.60.7.709.
[] Kessler R, Berglund P, Demler, Jin, R., Merikangas,K.R. & Walters, E.E. (2005) Lifetime prevalence and age-of-onset distributions of dsM-IV disorders in the national comorbidity survey Replication. Archives of General Psychiatry 62: 593-602. doi: 10.1001/archpsyc.62.6.593.
[] Association for Young People's Health: Key Data on Young People 2021.
[] Public Health England, The mental health of children and young people in England, December 2016.
[] Blackpool Council School Health Education Unit (SHEU) Health and Well-being of Young People in Blackpool, 2017 and 2019.
[] PHE Profile, Child and Maternal Health, Child Health Profiles. Reported numbers are rounded to the nearest 5.
[] Royal College of Psychiatrists. Self-harm, suicide and risk: helping people who self-harm. College Report CR158, June 2010.
[] OHID Public Health Profile, Children and Young People's Mental Health and Wellbeing, Identification of need. Reported numbers are rounded to nearest 5.
[] National Child Mortality Database (NCMD) (2021) Suicide in Children and Young People: National Child Mortality Database Programme Thematic Report - Data from April 2019 to March 2020.
[] OHID, Public Health Outcomes Framework / ONS Suicides in the UK statistics.
[] University of Manchester, Suicide by Children and Young People, National Confidential Inquiry into Suicide and Homicide by People with Mental Illness (NCISH). Manchester: 2017.
[] Office for Health Improvement and Disparities (OHID), Wider Impacts of COVID-19 on Health (WICH) monitoring tool. Accessed 4th February 2021 (data to September 2021).
[] Odd, D., Williams, T., Appleby, L., Gunnell. D. & Luyt, K. (2021) Child suicide rates during the COVID-19 pandemic in England. Journal of Affective Disorders Report, 6(Dec 2021), 100273. https://doi.org/10.1016/j.jadr.2021.100273.